Getting a new metabolic diagnosis often feels incredibly overwhelming for families. First of all, you might be desperately searching for the exact difference between type 1 and type 2 diabetes. As a medical doctor, I hear this anxious question from confused patients every single week in my clinic.
Both of these conditions are serious, chronic diseases that cause dangerously high blood sugar. However, they are actually fundamentally different illnesses. Furthermore, their underlying physiological causes and daily medical treatments look absolutely nothing alike.
Consequently, deeply understanding your specific condition is the very first step toward reclaiming your long-term health. Therefore, I will break down the complex medical science into simple, plain English for you today. Let’s clearly explore the true causes, symptoms, and life-saving treatments together right now.
TL;DR Summary Box
First of all, both conditions cause dangerously high blood sugar. However, the root causes and daily treatments differ entirely. Here is the quick medical bottom line:
- The Root Cause: In type 1, your immune system actively destroys your pancreas, so it produces zero insulin. On the other hand, type 2 develops from severe insulin resistance. Your body still makes insulin, but your cells stubbornly ignore it.
- Daily Treatment: Consequently, type 1 absolutely requires daily synthetic insulin injections to survive. In contrast, you can frequently manage type 2 using a healthy diet, regular exercise, and daily oral pills like Metformin.
- Prevention & Reversal: You simply cannot prevent type 1 diabetes. Furthermore, it currently has no cure. Conversely, you can often prevent type 2 entirely. Most noteworthy, losing significant weight can even put type 2 into long-term remission.
- Symptom Onset: Both cause extreme thirst, frequent urination, and severe fatigue. However, type 1 symptoms hit you incredibly fast and aggressively. Meanwhile, type 2 sneaks up silently over many years.
What Is Type 1 Diabetes?
Just last month, I sat down with a young patient named Liam, his question was “What is type 1 diabetes?” He suddenly developed severe type 1 diabetes symptoms out of nowhere. Therefore, I had to explain exactly what was happening inside his body. First of all, type 1 diabetes is strictly an autoimmune disease.
For some unknown reason, your body’s immune system makes a massive mistake. Specifically, it heavily attacks and completely destroys the beta cells inside your pancreas. Because these cells die, your pancreas completely stops producing insulin. Naturally, insulin acts like a vital chemical key.
It unlocks your cells so blood sugar can enter and provide your daily energy. As a result of this internal attack, sugar builds up rapidly in the bloodstream. Furthermore, you simply cannot prevent this specific condition with a good diet.
Genetics and certain environmental triggers cause the initial immune system failure. Consequently, Liam and other type 1 patients must rely on lifelong medical support. Namely, they must inject synthetic insulin every single day to survive. Also, they must carefully monitor their blood sugar around the clock.
What Is Type 2 Diabetes?
On the other hand, what is type 2 diabetes exactly? First, you should know that type 2 diabetes mellitus represents the most common diabetes type globally. In fact, it accounts for nearly 95% of all adult cases. Unlike the sudden autoimmune attack in type 1, this condition develops very slowly.
Specifically, your pancreas usually still makes insulin in the beginning. However, your body’s cells become incredibly stubborn and ignore the insulin signals. Medical professionals call this stubbornness insulin resistance. Because your cells resist the chemical key, sugar cannot enter them easily.
Therefore, sugar stays trapped in your bloodstream, heavily raising your overall glucose levels. Consequently, your pancreas desperately pumps out even more insulin to force the sugar into your cells. Over many years, your overworked pancreas simply wears out.
Eventually, it cannot produce enough insulin to keep up with the high demand. Most noteworthy, heavy lifestyle factors directly drive this disease. For example, carrying excess belly fat, living a highly inactive lifestyle, and eating poor diets vastly increase your risk. Still, strong family genetics also play a major role in your diagnosis.
Main Difference Between Type 1 and Type 2 Diabetes
If you want the key difference between type 1 and type 2 diabetes, look directly at the pancreas. In type 1, the pancreas produces zero insulin because of immune system damage. Thus, the insulin factory completely shuts down.
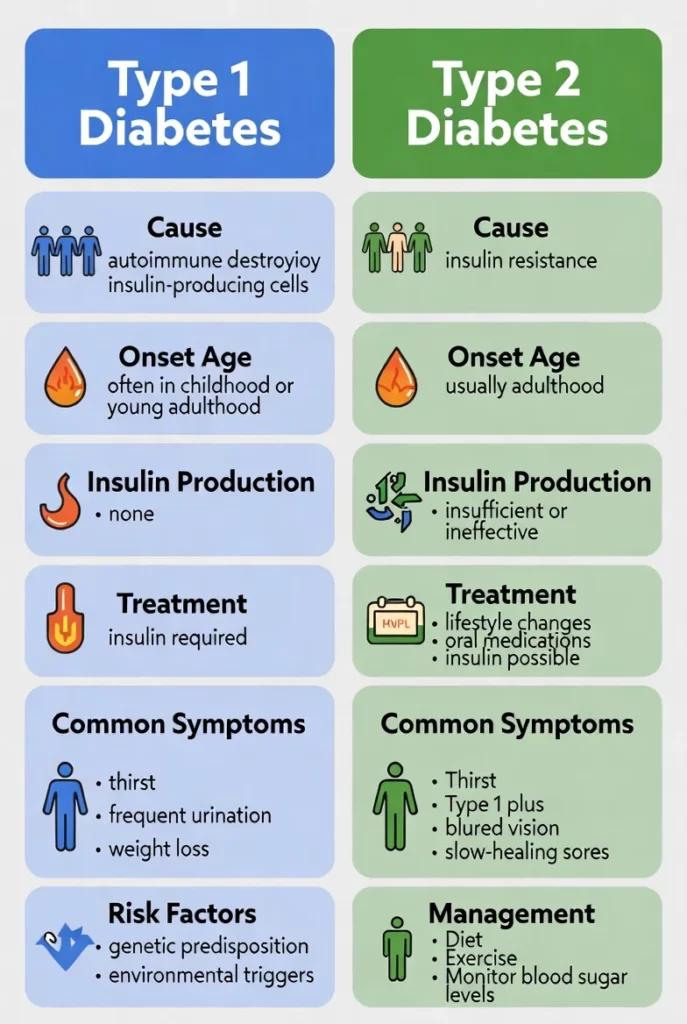
Conversely, in type 2, the pancreas still works, but the body actively rejects the insulin. Essentially, the factory produces the keys, but the locks on your cells are totally jammed. Therefore, the main difference lies entirely in the root functional cause.
Another major difference involves prevention. You simply cannot prevent type 1 through early lifestyle changes. However, you can frequently prevent or significantly delay type 2 through healthy eating and regular exercise.
Type 1 vs Type 2 Diabetes Comparison Chart
To illustrate the clinical facts clearly, here is a helpful type 1 vs type 2 diabetes chart. You can easily compare the distinct medical features side-by-side.
| Feature | Type 1 Diabetes | Type 2 Diabetes |
| Primary Cause | Autoimmune attack on pancreas | Insulin resistance & lifestyle |
| Insulin Production | None (pancreas cells destroyed) | Still produced, but ineffective |
| Prevention | Cannot be prevented currently | Often preventable via lifestyle |
| Typical Onset Age | Childhood or young adulthood | Usually adulthood (but dropping) |
| Daily Treatment | Strict daily insulin injections | Diet, pills, or sometimes insulin |
Type 1 vs Type 2 Diabetes Symptoms
Next, let’s explore the crucial difference between type 1 and type 2 diabetes symptoms. Both share very similar warning signs due to high blood sugar. For instance, frequent urination and extreme thirst happen in both conditions.
Also, extreme fatigue and blurry vision commonly affect patients in both groups. However, the exact timeline of these symptoms differs drastically. Specifically, type 1 diabetes symptoms hit you incredibly fast and severely.
A perfectly healthy teenager might fall dangerously ill in just a few short weeks. Furthermore, sudden, unexplained weight loss happens rapidly because the body aggressively starves without insulin. Thus, the clinical onset feels very dramatic and scary.
In contrast, type 2 symptoms sneak up on you silently over many years. Many people feel completely normal and naturally ignore the subtle physical changes. Therefore, doctors often discover the disease purely by accident during routine blood work.
Treatments: Type 1 vs Type 2 Diabetes
Therefore, we must thoroughly compare the basic treatments for type 1 and type 2 diabetes. As a physician, I spend a massive amount of time explaining the vital difference between type 1 and type 2 diabetes treatments. Consequently, you need to understand exactly how doctors manage each condition daily.
Type 1 Diabetes Treatment Strategies
First of all, treating type 1 strictly requires synthetic insulin. Because your pancreas produces zero insulin naturally, you absolutely must inject it. Otherwise, you will face life-threatening complications within days. Therefore, this chemical dependency never goes away.
Additionally, patients use multiple daily injections or wear an automated insulin pump. . Furthermore, they heavily rely on continuous glucose monitors to track their blood sugar safely. You basically become your own pancreas 24/7.
Type 2 Diabetes Medication and Lifestyle
On the other hand, type 2 treatment focuses heavily on fighting insulin resistance. Consequently, lifestyle changes serve as your primary, most powerful medicine. By losing significant weight and exercising vigorously, you directly heal your stubborn cells.
Furthermore, many patients ask me, does type 2 diabetes require insulin? Honestly, it usually does not initially. First, doctors prescribe oral medications like Metformin. This pill powerfully stops your liver from dumping excess sugar into your bloodstream.
In addition, we frequently prescribe modern injectable drugs like GLP-1 agonists. These amazing medications slow down your digestion and strongly suppress your appetite. Consequently, patients lose massive amounts of weight and drastically lower their A1C naturally.
Also, doctors use SGLT2 inhibitors to literally flush extra blood sugar out through your urine. However, if you ignore your diet for decades, your pancreas will eventually fail entirely. At that late stage, you will definitely require daily insulin injections to survive.
Type 1 vs Type 2 Diabetes Glucose Levels
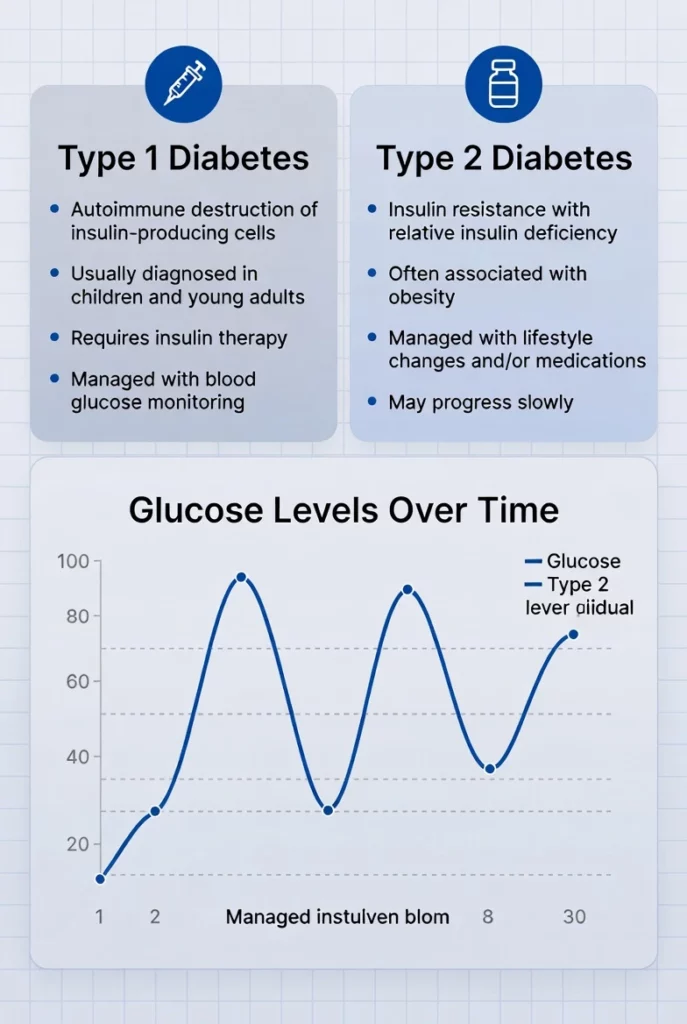
When discussing type 1 vs type 2 diabetes glucose levels, the core targets remain quite similar. Ultimately, doctors want both groups to maintain safe blood sugar ranges. However, the extreme daily fluctuations look very different.
Because type 1 patients lack natural insulin entirely, their levels can swing wildly and dangerously. They face a very high risk of severe low blood sugar (hypoglycemia) from synthetic insulin doses. Thus, they require constant daily vigilance.
Meanwhile, type 2 patients usually experience a slow, chronic elevation in daily blood sugar. While they can experience dangerous spikes, their levels tend to remain much more stable if they manage their daily diets well.
How to Know If You Have Type 1 or Type 2 Diabetes
Next, how to know if you have type 1 or 2 diabetes remains a very critical question. Specifically, doctors cannot simply guess based on your age or weight. Instead, we run highly advanced blood panels to find the exact root cause.
If you wonder how do I know if I am type 1 or 2 diabetic, we check your autoantibodies. In type 1, your blood heavily contains specific immune system markers like GAD65. These completely prove an autoimmune attack is actively destroying your pancreas.
Additionally, we frequently run a C-peptide test. This simple blood test accurately measures exactly how much natural insulin your pancreas still produces. If your C-peptide is effectively zero, you definitively have type 1 diabetes.
Are You Born With Type 1 or Type 2 Diabetes?
Many worried parents frequently ask, are you born with type 1 or 2 diabetes? First of all, true neonatal diabetes is incredibly rare. You are almost never born with active, dangerously high blood sugar on day one.
However, you absolutely inherit a strong genetic risk for both types. Specifically, type 1 requires certain genetic markers combined with a random viral trigger later in childhood. Conversely, type 2 genetics strongly dictate how easily you develop severe insulin resistance as an adult.
Is Type 1 or Type 2 Diabetes More Common?
So, is type 1 or type 2 diabetes more common? Type 2 absolutely dominates the global statistics. In fact, type 2 accounts for nearly 90% to 95% of all diagnosed cases in the United States today.
Meanwhile, type 1 remains comparatively rare overall. It only makes up roughly 5% to 10% of the total diabetic population. Consequently, public health campaigns heavily focus on preventing type 2 through massive lifestyle interventions and diet changes.
Which Is Worse: Type 1 or Type 2 Diabetes?
Patients often ask me bluntly in the exam room, which is worse type 1 or 2 diabetes? Truly, comparing them is very difficult. Both conditions are incredibly dangerous if you leave them untreated and ignored.
If you ask which is more deadly type 1 or 2 diabetes in the short term, type 1 definitely wins. Without immediate daily insulin, a type 1 patient will quickly fall into a fatal coma. Therefore, it presents a constant, acute daily danger.
However, which is more serious type1 or type2 diabetes over a lifetime? Type 2 frequently kills people silently over decades. Because patients ignore the mild symptoms, they secretly develop massive heart disease, kidney failure, and strokes. Both demand your ultimate respect.
Can Type 2 Diabetes Be Reversed?
Can type 2 diabetes be reversed? This is the most exciting topic I discuss with my clinical patients. Last year, I watched a patient named Robert completely reverse his type 2 diagnosis simply by losing 40 pounds naturally.
Technically, we call this “remission” rather than a true cure. By eating a strict, low-carbohydrate diet and lifting heavy weights, Robert completely restored his insulin sensitivity. Thus, he currently maintains totally normal blood sugar without any medication. You can absolutely achieve this too.
Is There a Type 3 Diabetes?
Recently, you might have wondered, is there a type 3 diabetes? Medical researchers increasingly use this unofficial term to accurately describe Alzheimer’s disease. Fascinatingly, scientists discovered that human brain cells can develop severe insulin resistance.
Consequently, when your vital brain cells cannot absorb sugar, they literally starve and die off. Therefore, preventing chronic insulin resistance might powerfully protect your memory and cognitive function as you age. Protecting your metabolism protects your brain.
How Does Type 2 Diabetes Affect the Body?
So, how does type 2 diabetes affect the body ultimately? High blood sugar acts exactly like toxic, crushed glass flowing freely through your delicate veins. Over time, this intense friction systematically destroys your microscopic blood vessels.
Consequently, you face terrible complications like permanent blindness, nerve death in your feet, and total kidney failure. Furthermore, your massive risk for severe heart attacks and sudden strokes skyrockets. You must strictly control your blood sugar to desperately protect your vital organs.
What Are the Symptoms of Type 1 and Type 2 Diabetes?
What are the symptoms of type 1 and type 2 diabetes fundamentally? They both powerfully trigger the classic “three P’s” of high blood sugar. First, you experience intense polyuria (frequent urination) day and night.
Second, severe polydipsia (excessive thirst) keeps you drinking water constantly. Finally, polyphagia (extreme hunger) happens because your cells aggressively starve. You will also heavily notice blurred vision and severe daily exhaustion affecting your daily life.
Frequently Asked Questions
What is the difference between type 1 and type 2 diabetes?
Type 1 is an unpreventable autoimmune disease that aggressively destroys your insulin-producing pancreas cells. In contrast, type 2 is an insulin resistance condition largely driven by unhealthy lifestyle choices, excess weight, and strong genetics.
Which is worse type 1 or type 2 diabetes?
Both conditions are terribly dangerous. Type 1 causes immediate, acute, life-threatening emergencies without synthetic insulin injections. Meanwhile, type 2 silently destroys your heart, delicate kidneys, and eyes over many years of high blood sugar.
Can type 2 diabetes be reversed?
Yes, you can frequently put type 2 into long-term clinical remission. By losing significant body fat, eating healthy whole foods, and exercising vigorously, your body can naturally regain normal insulin sensitivity.
Is type 1 or type 2 diabetes more common?
Type 2 is vastly more common globally. It officially accounts for roughly 90% to 95% of all adult medical cases. Meanwhile, type 1 only represents about 5% of the total diabetic population.
Does type 2 diabetes require insulin?
Usually, it does not require insulin in the early disease stages. Doctors primarily use diet changes and daily oral medications like Metformin. However, severe, long-term cases eventually destroy the pancreas entirely, making daily insulin absolutely necessary.
Conclusion
In conclusion, understanding the true difference between type 1 and type 2 diabetes completely eliminates your fear. Ultimately, both conditions require your serious daily attention and proper medical care. However, their core treatments look vastly different.
First of all, if you have type 1, your immune system made a permanent mistake. Therefore, your pancreas produces no insulin, and you absolutely need daily synthetic injections to survive.
On the other hand, type 2 develops slowly from severe insulin resistance. Consequently, you can frequently manage or even completely reverse it through powerful lifestyle changes. By losing weight and exercising, you force your cells to work normally again.
Most importantly, never try to diagnose yourself at home. Instead, you must visit a qualified doctor for proper blood testing. We have amazing modern tools to pinpoint your exact condition instantly.
Evidence-Based References:
- American Diabetes Association (ADA) – Diagnosis and Classification of Diabetes
- Centers for Disease Control and Prevention (CDC) – Type 1 vs Type 2 Diabetes
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
- Mayo Clinic – Diabetes Types and Treatments
- World Health Organization (WHO) – Diabetes Overview

