Facing a surgical recommendation for a limb or toe is an incredibly heavy emotional burden for any family. You might feel scared when searching for answers online about survival rates and long-term outcomes. Many people naturally wonder, why do diabetics die after amputations? It is important to understand that the surgery itself is rarely the cause of death. Instead, amputation serves as a clinical marker for how advanced the systemic effects of diabetes have become in the body.
While the statistics can seem frightening, they do not tell your specific story. As a medical professional, I have sat with many patients navigating this exact crossroad. In my clinical experience, focusing on heart health and kidney function after surgery is just as vital as the wound care itself. Let’s look at the actual medical reasons behind these risks and how you can take control of your recovery.
TL;DR: The Essentials
- Amputation is a Marker: It indicates advanced vascular and nerve damage.
- Main Risks: Heart disease and kidney failure are the primary drivers of mortality.
- Survival Factors: Age, mobility, and early intervention significantly impact the outlook.
- Prevention Works: Consistent foot checks and blood sugar management save lives.
Why Do Diabetics Get Amputations in the First Place?
Diabetes affects the entire body, but the feet are particularly vulnerable. Over time, high blood sugar levels damage the tiny blood vessels and nerves. This leads to two primary issues: peripheral neuropathy and peripheral arterial disease (PAD). Peripheral neuropathy causes a loss of sensation. You might step on a tack or develop a blister and never feel it. Because you can’t feel the injury, it remains untreated. Meanwhile, PAD reduces blood flow to the area.
Without proper blood flow, the body cannot deliver the oxygen and immune cells needed to heal a wound. A small scrape can quickly turn into a deep diabetic foot ulcer. If the bone becomes infected (osteomyelitis), an amputation may become necessary to stop the spread of rot.
Why Do People Die After Amputations (Diabetes vs. Non-Diabetes)?
When comparing patients, those with diabetes often face higher risks than those losing a limb due to trauma. This is because trauma patients usually have healthy internal organs. In contrast, diabetes is a systemic illness. The same process that damages the feet also damages the heart and kidneys. Doctors often view an amputation as a “stress test” for the entire body. It reveals the extent of underlying cardiovascular strain.
While you can die from getting your leg amputated due to surgical complications, this is rare. Modern anesthesia and surgical techniques have made the procedure itself quite safe. The real danger lies in the body’s fragility before the surgery even begins.
Why Do Diabetics Die After Amputations? (Root Causes Explained)
So, why do diabetics die after amputations if the surgery is successful? The answer involves the “domino effect” of chronic health issues. Once a limb is removed, the body must work much harder to heal and move.
Severe Infection and Sepsis
If the infection isn’t caught early, bacteria can enter the bloodstream. This leads to sepsis, a life-threatening inflammatory response. Even after surgery, a weakened immune system might struggle to fight off secondary infections like pneumonia.
Advanced Cardiovascular Disease
Most diabetic patients requiring amputation also have significant blockages in their heart arteries. The physical stress of surgery and the subsequent rehabilitation can strain a weak heart. Heart attacks remain a leading cause of post-operative mortality.
Chronic Kidney Disease (CKD)
The kidneys are the body’s filters. Diabetes often causes these filters to fail. Patients with both diabetes and kidney failure have the hardest time recovering. Their bodies struggle to balance fluids and electrolytes during the healing process.
What Is the Survival Rate for Diabetic Amputations?
Statistics often show that the five-year survival rate for diabetic amputees is lower than many forms of cancer. Your individual health profile matters more than a general average.
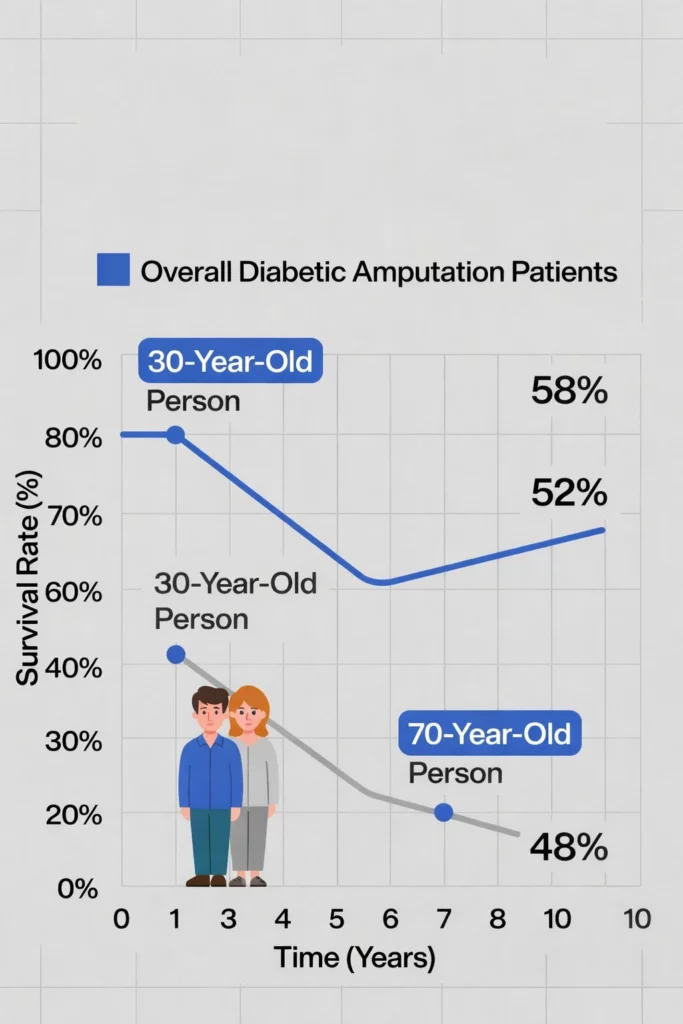
Lower-level procedures, like a toe or foot removal, generally have much better outcomes. Above-the-knee amputations are more taxing on the cardiovascular system. This is because it takes much more energy to walk with a prosthetic leg than a prosthetic foot.
| Amputation Level | 1-Year Survival (Approx) | 5-Year Survival (Approx) |
| Toe / Partial Foot | 90% | 70% |
| Below the Knee | 70% – 80% | 40% – 50% |
| Above the Knee | 50% – 60% | 20% – 30% |
How Long Do Diabetics Live After Amputations?
There is no “timer” that starts after surgery. Life expectancy varies wildly based on post-operative care. Some patients live for decades after an amputation, especially if they use it as a wake-up call to manage their health. Success depends heavily on mobility. Patients who engage in physical therapy and stay active tend to live much longer. Inactivity leads to muscle wasting and further heart strain.
Staying upright and moving is the best medicine for longevity. I recall a patient, a former teacher, who lost her foot but was determined to play with her grandkids. She followed her rehab plan religiously and improved her diet. Five years later, her heart was actually stronger than it was before the surgery.
What Is the Life Expectancy of a Person With an Amputated Foot?
Losing a foot is a major life change, but it is not a death sentence. In fact, partial foot amputations often have a very positive prognosis. The goal here is to preserve as much “functional length” as possible.
The life expectancy of a person with an amputated foot depends on preventing the next wound. If you protect your remaining foot, you can maintain a high quality of life. High-quality prosthetic inserts can make walking almost normal again.
What Is the Life Expectancy of a Diabetic Foot Ulcer?
This is a common question, but it’s a bit of a misnomer. A foot ulcer itself doesn’t have a life expectancy, but its presence is a warning sign. It signals that the body’s circulation is significantly compromised.
Studies suggest that people with active ulcers have a higher mortality risk than those without them. This is because the ulcer is a “window” into the health of your arteries. If a foot wound won’t heal, your heart vessels may also be narrowed.
What Happens If You Don’t Amputate a Leg in Diabetes?
Choosing surgery is terrifying, but avoiding it when medically necessary is often more dangerous. If you don’t amputate a severely infected leg, the infection will likely spread to the bone (osteomyelitis).
Eventually, the dead tissue (gangrene) releases toxins into the blood. This leads to organ failure and death within days or weeks. In these cases, amputation is actually a life-saving intervention. It removes the source of the poison so the rest of the body can survive.
How Dangerous Is the Amputation Surgery Itself?
Many people ask, how many hours does it take to amputate a leg? Generally, the procedure takes between one and three hours. It is a standard surgery that most vascular or orthopedic surgeons perform frequently. The primary risks during surgery are related to anesthesia. Because many diabetics have heart issues, the anesthesiologist must be very careful. However, with modern monitoring, the risk of dying on the operating table is extremely low.
Why Reddit Stories About Diabetic Amputations Can Be Misleading
If you search for “why do diabetics die after amputations Reddit,” you will find many heartbreaking stories. While these experiences are real, they are often subject to “selection bias.” People rarely post on Reddit to say their recovery was boring and successful.
Social media tends to highlight the most dramatic or tragic cases. Population-level data shows a much broader range of outcomes. Do not let an anonymous internet thread dictate your hope for the future. Every patient’s biology is unique.
Why UK and US Statistics May Look Different
You might notice different data if you search “why do diabetics die after amputations UK.” Health systems handle diabetic foot care differently across the globe. The UK’s NHS has a very structured “multidisciplinary foot team” approach.
In the US, care can be more fragmented depending on your insurance. However, the medical technology and surgical expertise in the US are world-class. Access to early screening is the biggest factor in preventing the need for surgery in the first place.
How to Prevent Diabetes Amputations
Prevention is always better than the best surgery. You can significantly lower your risk of ever needing an amputation by following a few daily habits. These small steps protect your “limbs and life.”
- Daily Foot Checks: Use a mirror to look at the bottoms of your feet every single night.
- Never Walk Barefoot: Even inside the house, wear supportive shoes or slippers to avoid small cuts.
- Manage Your A1c: Keeping blood sugar in your target range allows your body’s natural repair systems to work.
- Stop Smoking: Smoking constricts blood vessels and is the fastest way to lose a limb in diabetes.
- Professional Care: See a podiatrist at least once a year for a professional sensation test.
Foot Care Checklist
- Check for redness, swelling, or blisters.
- Wash feet in lukewarm (not hot) water.
- Dry thoroughly, especially between the toes.
- Apply moisturizer to the tops and bottoms (but not between toes).
- Trim toenails straight across.
When to Seek Immediate Medical Care
If you have diabetes, you should never “wait and see” with a foot wound. Small problems become big problems overnight. Contact your doctor immediately if you notice:
- A wound that has not started healing in 48 hours.
- Pus or drainage on your socks.
- A foul odor coming from a foot sore.
- The skin turning black, blue, or bright red.
- Fever, chills, or unexplained confusion.
Key Takeaway for Patients and Families
It is natural to feel overwhelmed when researching why do diabetics die after amputations. However, remember that an amputation is often the beginning of a new phase of care, not the end of the road.
By focusing on heart health, maintaining mobility, and performing daily foot checks, you can defy the statistics. You have the power to influence your recovery. Work closely with your medical team, stay active, and keep a close eye on your “good” foot to ensure it stays that way.
Frequently Asked Questions
How long is the hospital stay after an amputation?
Most patients stay in the hospital for 5 to 10 days. This allows doctors to monitor the incision for infection and ensure your pain is managed. You will likely transition to a rehabilitation center afterward to learn how to move safely.
Can you drive after losing a foot?
Yes, many people return to driving. If you lose your right foot, you may need to have your vehicle modified with a left-foot gas pedal. If it is your left foot and you drive an automatic, you may not need any changes at all.
Is phantom limb pain a sign of a problem?
No, phantom pain is very common. It happens because the brain still expects to receive signals from the missing limb. It usually fades over time and can be managed with specific medications or “mirror therapy.”
How soon can I get a prosthetic leg?
Usually, the limb needs to heal and the swelling must go down first. This typically takes 2 to 6 months. During this time, you will work with a prosthetist to ensure the best fit for your new limb.
Does insurance cover diabetic shoes?
In the US, Medicare and many private insurance plans cover one pair of extra-depth “diabetic shoes” and inserts per year. This is a critical preventive tool that you should discuss with your podiatrist.
Conclusion:
Facing the reality of a diabetic amputation is undoubtedly one of the most challenging experiences a patient or family can endure. It is easy to get lost in the statistics and wonder, why do diabetics die after amputations? However, as we have explored, the surgery itself is a tool used by surgeons to stop a life-threatening crisis. The path toward a long and fulfilling life after surgery depends on looking beyond the surgical site and focusing on the whole body.
The most critical window for recovery is the first twelve months following the procedure. During this time, your focus should shift toward protecting your heart and your remaining limb. Mortality risks are not set in stone; they are heavily influenced by how well we manage blood pressure, cholesterol, and kidney health. When you treat the underlying systemic issues, you change the narrative of your recovery.