Recognizing the warning signs of a sudden drop in glucose is one of the most essential skills for protecting your metabolic health. Low Blood Sugar Symptoms can appear quickly, whether you live with diabetes or occasionally experience sudden energy crashes, as your body signals that its primary fuel source is running low.
Understanding these changes early can help you act fast and prevent serious, potentially life-threatening complications. Low blood sugar (hypoglycemia) occurs when glucose levels drop below normal, typically under 70 mg/dL.
Common symptoms include shakiness, sweating, dizziness, confusion, and rapid heartbeat. If untreated, it can lead to severe complications such as fainting or seizures, making early recognition and treatment essential. To maintain your health, you must quickly identify these low blood sugar symptoms before they escalate.
Below, we break down exactly what these signs look like across different age groups, why they happen, and the exact steps you need to take to stabilize your system immediately.
What Are Low Blood Sugar Symptoms?
When your bloodstream lacks adequate glucose, your brain and organs essentially begin to starve. Because your brain relies almost exclusively on this sugar for energy, a drop in levels triggers an immediate panic response from your central nervous system.
If you are wondering what are the symptoms of low blood sugar, they generally fall into two categories: mild-to-moderate physical reactions and severe neurological impairments. Initially, your body releases adrenaline to forcefully release stored glucose from your liver, which causes the classic physical jitters.
As the condition worsens, what are the symptoms of low blood sugar transitioning into cognitive failures? Your brain begins shutting down non-essential functions to conserve its remaining fuel, leading to confusion, slurred speech, and extreme lethargy.
Symptoms When Blood Sugar Is Low
The specific symptoms when blood sugar is low can vary wildly from person to person. While one individual might become intensely irritable—often referred to as being “hangry”—another might simply become very quiet and pale.
It is crucial to understand these low blood sugar symptoms and signs as a progressive timeline. What starts as a mild headache or a slightly racing heart can quickly snowball into double vision and severe physical weakness within a matter of minutes.
Never ignore a sudden, unexplained shift in your physical or emotional state, especially if you have not eaten in several hours.
Low Blood Sugar Symptoms in Adults
General low blood sugar symptoms in adults typically manifest as a sudden drop in productivity or focus. Adults frequently mistake early causes of hypoglycemia for stress, exhaustion, or needing another cup of coffee.

However, unlike standard fatigue, a glucose crash feels highly urgent. You might notice your heart pounding against your chest, intense anxiety, or a tingling sensation around your lips and tongue. If you experience these signs, testing your levels using a reliable blood glucose monitor is the safest first step.
Low Blood Sugar Symptoms in Kids
Identifying low blood sugar symptoms in kids is exceptionally challenging because young children often lack the vocabulary to describe how they feel. Instead of saying they feel dizzy, a toddler might suddenly throw an uncharacteristic tantrum or refuse to walk.
Parents should watch for sudden paleness, excessive crying, nightmares during sleep, or complaints of a “tummy ache.” If a normally active child becomes suddenly lethargic, sweaty, and unresponsive to questions, you must treat the situation as a potential glucose emergency immediately.
Low Blood Sugar Symptoms During Pregnancy
Metabolic changes during gestation require careful monitoring. Low blood sugar symptoms pregnancy episodes are actually quite common, especially during the first trimester as the growing baby continuously draws glucose from the mother’s bloodstream.
Expectant mothers frequently experience sudden nausea, dizziness, and extreme exhaustion when their levels dip.
Low Blood Sugar Symptoms Without Diabetes
You do not need a metabolic disease to experience a dangerous glucose crash. Many people experience low blood sugar symptoms without diabetes, a condition broadly referred to as non-diabetic hypoglycemia.
If you are investigating what causes low blood sugar without diabetes, the most common culprit is reactive hypoglycemia. This happens when you eat a highly processed, sugary meal, causing your pancreas to over-produce insulin and violently crash your glucose a few hours later.
Other causes include excessive alcohol consumption on an empty stomach, severe liver disease, or eating disorders.
Diabetes Low Blood Sugar Symptoms
For those with metabolic disease, navigating diabetes low blood sugar symptoms is a daily reality. The medications used to manage the condition, particularly synthetic insulin or sulfonylureas, are designed to aggressively lower glucose.
If a patient takes too much medication, skips a meal, or exercises harder than usual, their levels will plummet. To understand this practically, I recently processed a clinical medical interview featuring a patient named Robert.
He described his type 1 diabetes low blood sugar symptoms not as textbook hunger, but as a sudden, overwhelming wave of panic and a racing heart while driving. His case study highlights that a diabetic low blood sugar symptoms episode can strike without warning, proving why keeping emergency glucose tabs in your car or bag is a matter of life and death.
High vs Low Blood Sugar Symptoms
Confusing a glucose spike with a sudden crash can lead to dangerous treatment errors. Understanding high vs low blood sugar symptoms ensures you take the correct corrective action immediately. High blood sugar (hyperglycemia) develops slowly over days, while a crash happens in minutes.
When comparing low blood sugar and high blood sugar symptoms, thirst and urination point to high levels, whereas sweating and shaking point to low levels. Review the comparison table below to memorize the critical differences between these two medical states.
| Symptom Category | Low Blood Sugar (Hypoglycemia) | High Blood Sugar (Hyperglycemia) |
| Onset Speed | Sudden and rapid (minutes) | Gradual and slow (days or weeks) |
| Skin Appearance | Pale, cold, and clammy | Flushed, dry, and warm |
| Physical Signs | Trembling, rapid heartbeat, dizziness | Extreme thirst, frequent urination |
| Mental State | Sudden confusion, irritability, anxiety | Lethargy, difficulty concentrating |
Physical Signs: Skin, Headaches, and More
Your body exhibits highly visible clues when it runs out of fuel. Observing low blood sugar symptoms on skin is often the easiest way to identify a crash in someone else. The skin typically loses its natural color, becoming extremely pale, grayish, and covered in a cold sweat.
Additionally, headaches low blood sugar connections are incredibly common. Because your brain is starving for its primary energy source, blood vessels often react by spasming or expanding. This creates a dull, throbbing pain at the front of the head that will not resolve with standard painkillers until glucose is restored.
What Happens When Blood Sugar Is Too Low?
When a patient asks, what happens when your sugar level is low, the physiological answer involves an emergency systemic shutdown. Your pancreas immediately stops releasing insulin and signals the liver to dump its emergency glycogen stores.
If those stores are depleted, your central nervous system begins to falter. Your vision blurs, motor skills degrade, and speech becomes heavily slurred. Without rapid intervention, this energy deficit causes the brain to misfire, leading to a complete loss of consciousness.
What Level of Low Blood Sugar Is Dangerous?
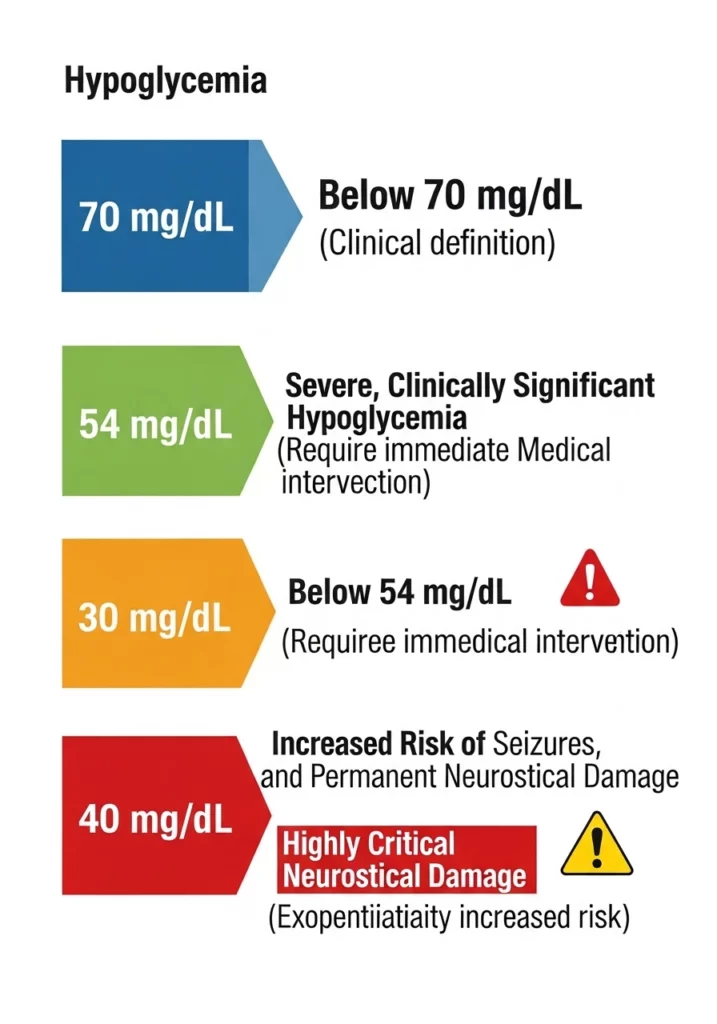
Defining exactly what level of low blood sugar is dangerous depends entirely on the individual’s baseline health. However, clinical guidelines generally define hypoglycemia as any reading consistently falling below 70 mg/dL.
Levels dropping below 54 mg/dL indicate severe, clinically significant hypoglycemia requiring immediate medical intervention. When readings fall below 40 mg/dL, the risk of seizures, coma, and permanent neurological damage increases exponentially.
What Is a Hypoglycemic Episode?
A “hypoglycemic episode query” refers to the active, symptomatic window when glucose drops below standard operational limits. An episode is not a disease itself, but rather an acute physiological event triggered by external factors like medication, diet, or exercise.
These episodes are categorized by severity. Mild episodes can be self-treated with food, while severe episodes render the patient incapacitated and entirely reliant on emergency assistance from a caregiver or paramedic.
Low Blood Sugar Causes
Understanding low blood sugar causes is the only way to prevent recurrent, dangerous episodes. For individuals managing diabetes naturally, the absolute most common cause is a mismatch between insulin medication and carbohydrate intake. If you inject a rapid-acting insulin but delay your meal by even thirty minutes, your glucose will inevitably crash.
Similarly, taking an oral sulfonylurea medication and then skipping breakfast creates a dangerous excess of circulating insulin. Physical activity also heavily influences your numbers. Exercise dramatically increases cellular insulin sensitivity, meaning your muscles rapidly absorb glucose directly from the bloodstream to fuel your workout.
If you do not consume a small carbohydrate snack before intense physical labor or a long run, you risk an exercise-induced crash. Furthermore, drinking alcohol on an empty stomach temporarily paralyses your liver’s ability to release its emergency glucose stores, making late-night hypoglycemia a massive risk.
For non-diabetics, extreme fasting, restrictive crash dieting, or underlying endocrine disorders like adrenal insufficiency can trigger these crashes. Additionally, gastric bypass surgery can alter how quickly food moves into the small intestine, leading to an exaggerated insulin response and subsequent glucose drop.
What to Do When Blood Sugar Is Low
Knowing exactly low blood sugar symptoms what to do during a crisis prevents a mild crash from becoming a hospital visit. The moment you feel shaky or confused, you must immediately stop any physical activity, sit down, and check your levels with a glucose monitor if one is available.
If you cannot test, treat the situation as a confirmed crash. Knowing low blood sugar symptoms how to fix quickly relies entirely on the clinical “15-15 Rule.” This proven medical protocol involves consuming exactly 15 grams of fast-acting carbohydrates and then waiting precisely 15 minutes before retesting your levels.
Immediate Food Interventions
Choosing what to eat when blood sugar is low dictates how quickly your brain recovers. You need pure, simple carbohydrates that require zero digestion to enter the bloodstream instantly. Avoid chocolate or baked goods, as their high fat content severely delays glucose absorption.
The most effective, rapid-acting options include:
- Chewing 3 to 4 pure glucose tablets.
- Drinking 4 ounces (half a cup) of fruit juice or regular, non-diet soda.
- Swallowing 1 tablespoon of pure honey or maple syrup.
Low Blood Sugar Treatment
Long-term low blood sugar symptoms treatment focuses on preventing the root cause of the drop. During a routine clinic visit last month, a patient named Sarah experienced repeated mid-morning crashes. By analyzing her continuous glucose monitor data, we discovered her basal insulin dose was simply too high, highlighting the need for continuous medical adjustments.
For severe emergencies where the patient is unconscious and cannot safely swallow juice, a caregiver must administer prescription glucagon. Glucagon is a synthetic hormone available as a pre-filled injection or a nasal spray (like Baqsimi) that forces the liver to instantly dump massive amounts of stored glucose into the blood.
Can You Die from Low Blood Sugar in Your Sleep?
A highly distressing but valid question is can you die from low blood sugar in your sleep. Nocturnal hypoglycemia is a profound risk, particularly for individuals taking long-acting insulin before bed.
Because you are asleep, you may sleep completely through the initial warning signs like sweating or shaking. In extremely rare, severe cases, prolonged and untreated nocturnal crashes can lead to “dead in bed syndrome,” a fatal cardiac arrhythmia triggered by the severe stress of an extended glucose deficit.
Related Conditions
Metabolic crashes rarely happen in a vacuum, and they frequently overlap with other cardiovascular issues. The physical sensation of a crash can closely mimic low blood pressure symptoms, as both cause intense dizziness, sudden fatigue, and visual disturbances when standing up too quickly.
Furthermore, experiencing high blood pressure and low blood sugar symptoms simultaneously is a massive stress event for the heart. The adrenaline released to combat the glucose crash physically constricts blood vessels, temporarily driving your blood pressure dangerously high while your energy levels plummet.
Frequently Asked Questions
What are 5 signs of low blood sugar?
The five most prominent early signs include sudden uncontrollable shakiness, cold clammy sweating, dizziness or lightheadedness, intense hunger, and sudden mental confusion or irritability. Recognizing these instantly allows for rapid treatment.
What happens when your sugar level is low?
When levels drop below normal, your brain becomes starved for energy. Your body releases adrenaline to access stored sugar, causing physical jitters. Eventually, cognitive functions begin to shut down, leading to slurred speech, blurred vision, and potentially fainting.
What to eat when blood sugar is low?
You must consume 15 grams of fast-acting, fat-free carbohydrates. The best options are 4 ounces of regular fruit juice, half a can of non-diet soda, one tablespoon of pure honey, or 3 to 4 medical glucose tablets.
What level of low blood sugar is dangerous?
Clinically, any reading below 70 mg/dL requires immediate treatment. Readings that drop below 54 mg/dL are considered dangerously severe, and numbers below 40 mg/dL present an immediate, critical risk of seizures and coma.
What is a hypoglycemic episode?
A hypoglycemic episode is a temporary, acute medical event where the glucose in your blood falls below the necessary threshold to fuel your body safely. It causes sudden physical and neurological distress until carbohydrates are consumed.
Conclusion
Recognizing a sudden drop in your glucose is a vital skill that protects your brain, heart, and long-term metabolic health. Whether you live with a formal diabetes diagnosis or simply experience reactive crashes after meals, your body will always give you warning signs.
Listening to those early cues like shakiness and sudden sweating can prevent a minor inconvenience from turning into a severe medical emergency. In my years of discussing metabolic health with patients, the most common mistake is simply being unprepared.
I always advise keeping a small tube of fast-acting glucose tablets or a juice box in your car, purse, or desk drawer at all times. This simple, inexpensive habit entirely removes the panic of a sudden crash, giving you immediate control over your physical safety and peace of mind.
Ultimately, if you experience recurrent hypoglycemic episodes, you must not ignore them or continuously self-treat without medical guidance. Schedule an appointment with your primary care physician or endocrinologist to investigate the root cause.
By adjusting your diet, tweaking your medications, and staying vigilant, you can comfortably live a full, active life without the constant fear of a sudden energy crash.
Evidence-Based References:
- American Diabetes Association (ADA) — Hypoglycemia (Low Blood Glucose)
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) — Low Blood Glucose (Hypoglycemia)
- Mayo Clinic — Hypoglycemia: Symptoms and causes
- Cleveland Clinic — Hypoglycemia (Low Blood Sugar)
- Centers for Disease Control and Prevention (CDC) — Low Blood Sugar (Hypoglycemia)

