Pregnancy brings a lot of sudden changes. Have you recently heard the term “gestational diabetes”? Maybe your doctor just mentioned it at your last checkup. You probably feel a little anxious right now. So, exactly what is gestational diabetes?
It is simply a blood sugar issue that pops up while you are expecting. Furthermore, it affects around 5% to 10% of all pregnancies in the United States. Because of this, you are certainly not alone. I recently sat down with a patient in her second trimester. She felt terrified after seeing her lab results.
I told her exactly what I tell all my patients: gestational diabetes, what is it? It is a temporary hurdle. You can manage it easily with the right tools. Most noteworthy, it usually goes away completely after you deliver your baby. Let us break down everything you need to know about what gestational diabetes in pregnancy is, from the early warning signs to the best diet plans.
TL;DR: What Is Gestational Diabetes?
First of all, it is a very common, temporary blood sugar condition that happens specifically during pregnancy. Placental hormones naturally block your body’s normal insulin, causing your blood sugar to rise.
Furthermore, most expecting mothers never feel any early warning signs. Therefore, your obstetrician will routinely test your blood sugar between weeks 24 and 28 of your pregnancy to keep you safe.
Finally, you can easily manage this condition if you test positive. As a result of eating a high-fiber diet, taking daily walks, and checking your blood sugar, you will protect your baby. Most importantly, the condition almost always disappears completely after you deliver.
- The Cause: Normal pregnancy hormones cause temporary insulin resistance.
- The Test: Doctors routinely screen for it at 24 to 28 weeks.
- The treatment: Daily blood sugar monitoring, balanced meals, and light exercise.
- The Outlook: Highly manageable, usually ending with a perfectly healthy baby and a safe delivery.
What Is Gestational Diabetes in Pregnancy?
During a normal pregnancy, your body changes rapidly. Your placenta grows to support your baby. First of all, this placenta releases a massive wave of hormones. These hormones help your baby develop safely. However, these same hormones block the action of the mother’s insulin.
We call this insulin resistance. Therefore, your body needs up to three times as much insulin to process blood sugar. When your pancreas cannot keep up with this heavy demand, your blood sugar rises. What type of diabetes is gestational diabetes? It is strictly linked to pregnancy, unlike Type 1 or Type 2.
What Causes Gestational Diabetes?
Many expecting parents sit in my office and ask, “What causes gestational diabetes?” They often blame themselves. Please do not do this. You did not cause this condition by eating a candy bar last week. First, pregnancy hormones drive this entire process.
Your placenta creates hormones like human placental lactogen. Consequently, these hormones naturally make your cells resist insulin. Second, your genetics play a massive role. If your parents or siblings have diabetes, your risk increases.
Furthermore, carrying extra weight before you get pregnant forces your body to work harder to use insulin. What is gestational diabetes caused by at its core? It is a heavy mix of unavoidable placental hormones, family history, and your body’s baseline insulin sensitivity. Due to these factors, your pancreas simply falls behind.
Is Gestational Diabetes Caused by the Father?
Fathers often ask me about their role in this diagnosis. Is gestational diabetes caused by the father? The short answer is no, but genetics do matter. The father does not directly cause the mother’s insulin resistance. However, the father provides half of the baby’s DNA.
Therefore, the father’s genes influence the placenta’s growth and hormone production. If the father has a strong family history of diabetes, he passes those genetic risk factors to the baby. As a result, the placenta might produce more insulin-blocking hormones. Still, we never blame the father for the mother’s GDM diagnosis.
Warning Signs of Gestational Diabetes
You might wonder how you will know if your blood sugar spikes. What is gestational diabetes symptoms like in real life? The tricky part is that most women feel absolutely nothing. Because the symptoms are so mild, you might confuse them with normal pregnancy fatigue.
However, you should watch for a few key warning signs of gestational diabetes. You might experience excessive thirst throughout the day. Also, you could notice extremely frequent urination, even more than usual for a pregnant woman.
Finally, blurred vision and intense fatigue serve as strong red flags. Since these warning signs of gestational diabetes stay hidden so well, routine medical screening becomes incredibly important. We do not wait for you to feel sick.
What Week Is the Gestational Diabetes Test?
Timing matters immensely in prenatal care. What week is the gestational diabetes test usually scheduled? We almost always test expecting mothers between weeks 24 and 28 of pregnancy. Why do we wait until the late second trimester?
Because this is exactly when your placenta reaches a size where it pumps out maximum hormones. Testing earlier usually misses the insulin resistance. If you have high-risk factors of type 2 diabetes, like a previous GDM diagnosis or a high BMI, we might test you during your very first prenatal visit. Otherwise, expect this crucial screening right around that 24-week mark.
What Is the Gestational Diabetes Test?
Because this is such a critical part of your prenatal care, we need to dive deep into the testing process. Patients always ask me, “What is the gestational diabetes test going to feel like?” We typically use a strict two-step process in the United States to ensure complete accuracy.
First of all, you need to understand that we are intentionally stressing your body’s insulin response. We give you a heavy dose of sugar and watch how quickly your pancreas reacts. Consequently, this tells us exactly how well you manage glucose.
Glucose Challenge Test
We start with the initial screening, called the glucose challenge test. You do not need to fast for this appointment. You will go to the lab and drink a very sweet, syrupy liquid containing exactly 50 grams of glucose. After you finish the drink, you wait exactly one hour.
Then, the phlebotomist draws your blood. If your blood sugar level comes back below 140 mg/dL, you pass. You do not have GDM. However, if your blood sugar spikes above that number, it signals a potential problem. Seems like your body struggles with sugar. Therefore, you must return for the second, more diagnostic step.
Oral Glucose Tolerance Test (OGTT)
If you fail the first screening, you move on to the oral glucose tolerance test (OGTT). This test is much more intense. First, you must fast completely for at least 8 to 14 hours before you arrive. We draw a baseline fasting blood sample immediately. Next, you drink a much stronger glucose liquid containing 100 grams of sugar.
Finally, we draw your blood three more times: at one hour, two hours, and three hours after drinking. If two or more of those specific blood draws show elevated numbers, we officially diagnose you with GDM. This diagnostic test gives us the final, undeniable proof of your insulin resistance.
Gestational Diabetes Blood Sugar Range
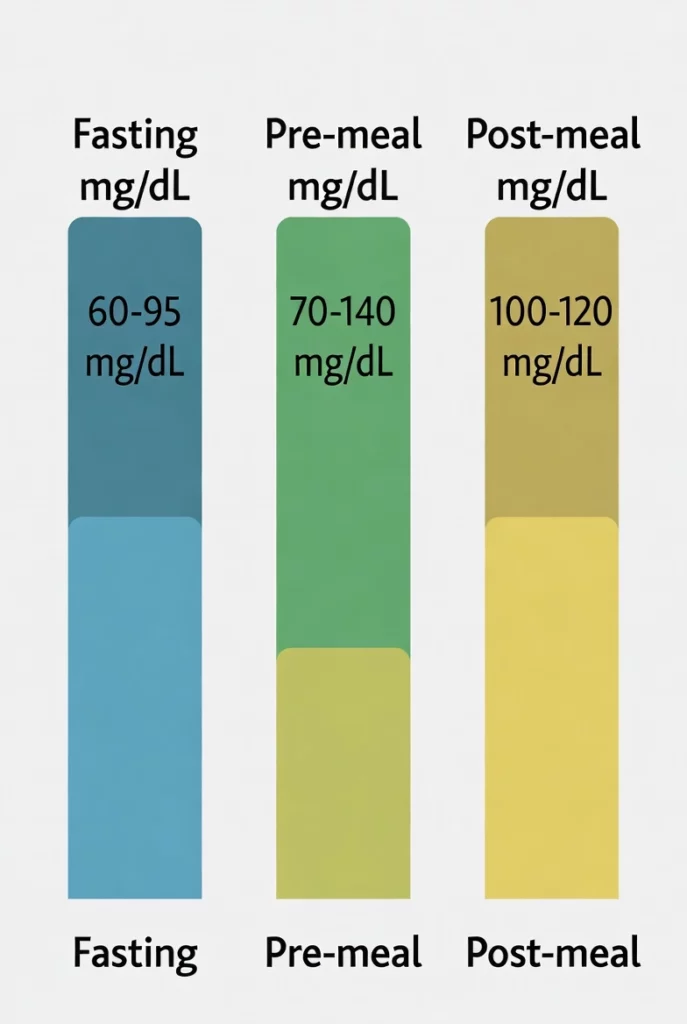
Once we establish a diagnosis, you must monitor your numbers at home. What are the gestational diabetes range targets for a healthy pregnancy? We keep these targets very tight to protect your baby.
With gestational diabetes, what is too high? Any fasting number over 95 mg/dL poses a risk. Below is a simple table showing the strict medical targets you need to hit daily.
| Testing Time | Normal Pregnancy Goal | GDM Diagnosis Threshold (OGTT) |
| Fasting (Morning) | Under 95 mg/dL | 95 mg/dL or higher |
| 1 Hour After Meal | Under 140 mg/dL | 180 mg/dL or higher |
| 2 Hours After Meal | Under 120 mg/dL | 155 mg/dL or higher |
What is considered gestational diabetes is any consistent pattern above these specific goals. Therefore, tracking your numbers daily becomes your most powerful tool for a safe delivery.
Treatment for Gestational Diabetes
Many women panic after receiving their diagnosis. However, you have many effective tools at your disposal. What is the treatment for gestational diabetes? First of all, it revolves around keeping your blood sugar completely stable. You must take an active role in your daily care.
Therefore, your treatment for gestational diabetes starts with routine monitoring. You will check your blood sugar levels using a small home meter. I recently taught a terrified patient how to use her new glucose monitor. She thought it would hurt terribly. However, within two days, she tested her blood four times daily with absolute confidence.
What is gestational diabetes treatment when diet and exercise fall short? If your numbers stay high, your obstetrician might prescribe insulin. You inject this safe medication to manually lower your blood sugar. It does not cross the placenta, so it keeps your baby perfectly safe.
Gestational Diabetes Diet
Food becomes your most powerful medicine right now. You do not need to starve yourself. Instead, you need a smart gestational diabetes diet. You must balance your carbohydrates with healthy proteins and fats. For example, eating a piece of plain toast will spike your sugar instantly.
Conversely, adding scrambled eggs and avocado to that toast slows down the sugar release. Consequently, your pancreas can easily handle the meal. Furthermore, you should eat three small meals and two to three snacks every single day. Skipping meals actually makes insulin resistance worse. Thus, eating consistently keeps your energy up and your numbers down.
Best Fruits for Gestational Diabetes
Many patients assume they must give up all fruit entirely. This is simply not true. So, what fruit is good for gestational diabetes? You just need to choose fruits packed with heavy dietary fiber. Because fiber slows down digestion, berries serve as your absolute best option.
Raspberries, blackberries, and strawberries provide fantastic sweetness without massive sugar spikes. Specifically, they pair perfectly with a handful of almonds. Additionally, crisp apples and hard pears work wonderfully. You should always eat the skin, as it contains all the crucial fiber. Finally, small oranges offer great vitamins, but always eat the whole fruit instead of drinking fruit juice.
How Does Gestational Diabetes Affect the Baby?
Mothers always ask me about their little ones first. How does gestational diabetes affect the baby? Because extra glucose crosses the placenta, your baby’s pancreas must produce extra insulin to handle it. As a result, this extra energy gets stored as fat. This leads to a condition called macrosomia, meaning a very large baby.
Consequently, delivering a large baby increases your risk of needing a C-section. Furthermore, high blood sugar can cause premature birth. After delivery, your baby’s own insulin levels might remain very high. Therefore, the newborn might experience sudden low blood sugar, known as newborn hypoglycemia, shortly after birth.
What Happens If Gestational Diabetes Is Not Controlled?
You absolutely must take your daily management seriously. What happens if gestational diabetes is left untreated? Ignoring your high blood sugar puts both you and your baby at severe risk. First of all, what is a complication of gestational diabetes for the mother?
You face a much higher risk of developing preeclampsia. This dangerous condition causes severe high blood pressure and threatens your life. What happens if gestational diabetes is not controlled throughout the third trimester? You might face birth trauma during a vaginal delivery. Because the baby grows too large, its shoulders can get stuck during birth.
Is Gestational Diabetes Dangerous?
Hearing about these complications sounds incredibly scary. Is gestational diabetes dangerous? Unmanaged high blood sugar certainly carries heavy risks. However, you hold the power to completely minimize these dangers.
If you monitor your numbers, eat well, and stay active, you face very little danger. In fact, most women with this condition deliver perfectly healthy, happy babies. Therefore, the real danger only exists if you ignore the diagnosis.
Does Gestational Diabetes Go Away?
You might wonder if you will need insulin forever. Does gestational diabetes go away? Yes, almost always. Once you deliver the baby and the placenta leaves your body, your hormones return to normal.
Usually, your blood sugar stabilizes within a few hours to a few days after childbirth. We will test your blood sugar again about six to twelve weeks postpartum. This ensures your insulin resistance has fully resolved.
However, you must remember one crucial detail. Having this temporary condition increases your future risk. Specifically, you have a much higher chance of developing Type 2 diabetes later in life.
How Can You Prevent Gestational Diabetes?
If you plan to get pregnant again, you can take action now. You cannot change your genetics, but you can change your lifestyle habits.
First, aim to reach a healthy weight before you conceive. Dropping even a few extra pounds improves how your body uses insulin. Also, adopt a balanced diet rich in vegetables, lean proteins, and whole grains.
Finally, build a strong exercise routine. Walking, swimming, or lifting light weights forces your muscles to absorb extra glucose. Consequently, this daily movement keeps your blood sugar perfectly balanced before your next pregnancy begins.
How Do You Manage Gestational Diabetes in Pregnancy?
Creating a daily routine makes everything easier. How do you manage gestational diabetes in pregnancy? You simply combine testing, eating, and moving into a predictable daily schedule.
First, test your fasting sugar immediately upon waking up. Next, take a protein-heavy best breakfast for diabetes . Afterward, take a brisk 15-minute walk. This gentle exercise burns off the morning carbohydrates instantly.
Throughout the day, drink plenty of water and never skip your snacks. Always bring your glucose monitor when you leave the house. By treating your daily management like a simple checklist, you remove the stress and protect your baby.
Frequently Asked Questions
What is gestational diabetes?
Gestational diabetes is a temporary type of diabetes that happens exclusively during pregnancy. Your pregnancy hormones block your body’s insulin. As a result, your blood sugar rises too high, requiring daily medical management.
What week is the gestational diabetes test?
Doctors usually schedule the gestational diabetes test between weeks 24 and 28 of your pregnancy. During this specific window, your placenta produces the highest amount of insulin-blocking hormones.
How does gestational diabetes affect the baby?
If left unmanaged, extra sugar crosses the placenta and makes the baby grow excessively large. Furthermore, the baby might experience dangerously low blood sugar immediately after birth.
Does gestational diabetes go away?
Yes, it almost always disappears immediately after you deliver your baby and the placenta. However, mothers who experience this condition face a higher risk of developing Type 2 diabetes later in life.
Is gestational diabetes dangerous?
It is dangerous only if you leave it completely unmanaged. If you follow your doctor’s diet plan and monitor your blood sugar daily, you can easily prevent complications and deliver a perfectly healthy baby.
Conclusion
In conclusion, finding out you have blood sugar issues during pregnancy feels overwhelming at first. However, when you finally understand exactly what gestational diabetes is, you quickly take back your power. Therefore, you do not need to panic.
Ultimately, this temporary condition requires your daily attention, but it certainly does not define your entire pregnancy experience. By simply monitoring your numbers, eating fiber-rich foods, and moving daily, you actively protect your baby. Furthermore, your healthcare team walks this entire journey with you.
In the end, managing your blood sugar successfully leads directly to a safe delivery and a perfectly healthy newborn. So, take a deep breath, strictly follow your doctor’s treatment plan, and focus on the beautiful reward waiting for you at the finish line.
Evidence-Based References:
- Centers for Disease Control and Prevention (CDC) — Gestational Diabetes Basics
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK) — What is Gestational Diabetes?
- Cleveland Clinic — Gestational Diabetes: Causes, Symptoms & Treatment
- Mayo Clinic — Gestational Diabetes Overview
- American College of Obstetricians and Gynecologists (ACOG) — Gestational Diabetes FAQ

