Have you noticed mysterious brown spots appearing on your shins lately? You are not alone. Diabetic dermopathy affects millions of Americans living with diabetes every single day.
These harmless patches often catch people off guard during their morning shower. You might wonder what causes them and whether they signal something serious.
Let us be honest—finding unexpected skin changes can feel unsettling. Your mind races with questions. Are these spots dangerous? Will they spread? Do they mean your diabetes is getting worse?
Fortunately, diabetic dermopathy itself causes no pain or health risks. However, these marks do tell an important story about your blood sugar control.
Think of them as visible reminders from your body. They indicate that tiny blood vessels have experienced stress over time. The good news? You hold significant power to prevent new spots from forming. Better glucose management makes a real difference. Simple skincare habits protect your legs effectively.
In this comprehensive guide, you will discover exactly what causes these shin spots. We will show you clear pictures for easy identification. You will learn proven strategies to protect your skin. Most importantly, you will understand when these marks warrant medical attention.
Ready to take control of your skin health? Let us dive deep into everything you need to know about diabetic dermopathy.
TL;DR
Diabetic dermopathy causes light or dark brown patches on the shins. This harmless condition affects many people with diabetes. The spots indicate underlying blood sugar issues. Treatment focuses on glucose control and skin protection. No specific cream removes these marks completely.
What Is Diabetic Dermopathy?
You might notice strange brown spots appearing on your lower legs. Diabetic dermopathy represents the most common skin finding in diabetes. These round or oval patches develop when small blood vessels change.
The condition affects up to 50% of diabetic patients. You will see them most often on the shins. The spots cause no pain or itching. They signal that diabetes affects your circulation. Early recognition helps you manage your overall health better.
What Does Diabetic Dermopathy Look Like?
These patches start as pink or red areas. They gradually turn light brown or reddish-brown. The spots measure 0.5 to 1 centimeter, typically. You will notice they appear round or oval. The surface remains smooth and slightly indented.
No scaling or crusting develops. The patches fade slowly over months. New ones may appear as old ones fade. Multiple spots often cluster on both shins. They look similar to age spots but appear earlier.
Diabetic Dermopathy Pictures and Visual Identification
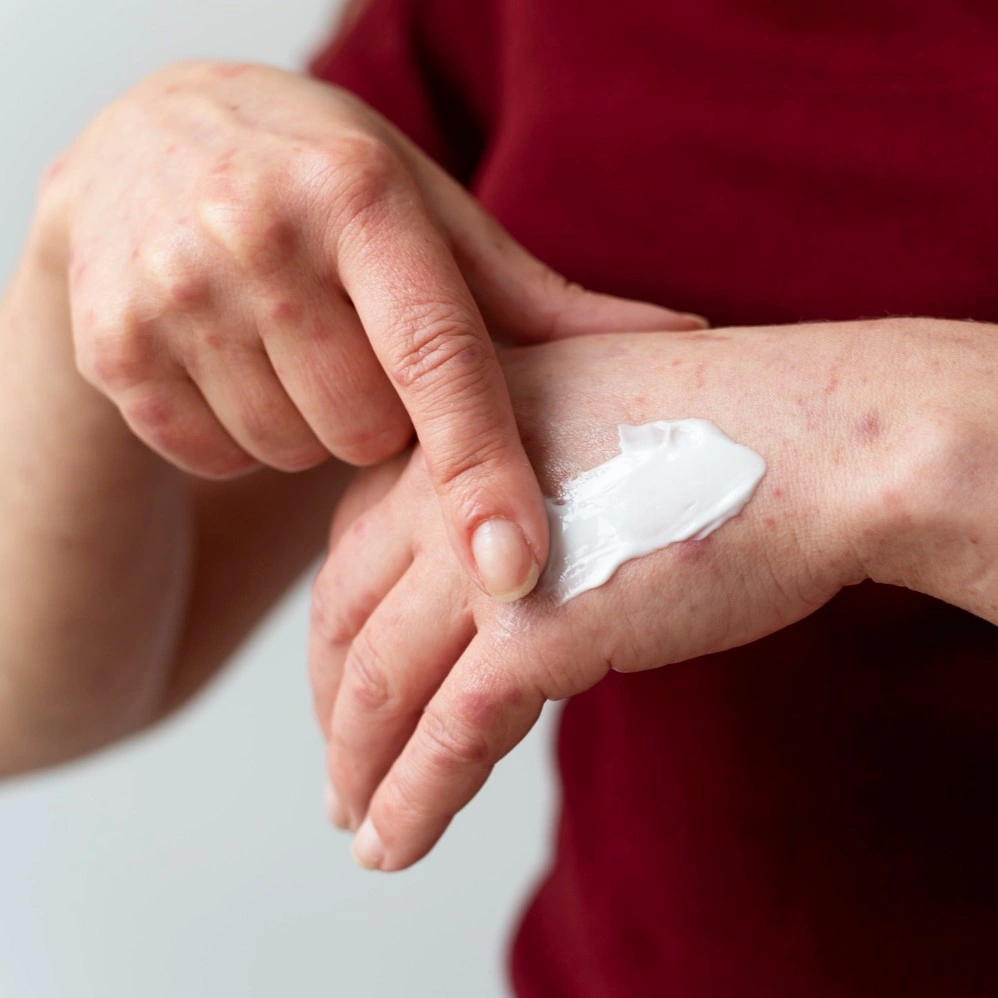
Visual recognition helps you track changes accurately. The spots appear symmetrically on both legs, usually. You will see them clearly against the normal skin tone. Early lesions look pink before turning brown. Advanced spots become darker and more defined.
The surrounding skin stays completely normal. No redness or swelling accompanies these marks. Photos help doctors monitor progression over time. You should document new spots with your smartphone. Compare images monthly to track changes.
Diabetic Dermopathy Symptoms
These patches cause absolutely no discomfort. You will not feel itching or burning sensations. The spots remain flat against your skin surface. No oozing or bleeding occurs. They do not interfere with daily activities.
Most people discover them accidentally while bathing. The cosmetic appearance bothers some individuals. However, medical intervention remains unnecessary. You should still mention them to your doctor. They indicate how well you control diabetes.
Early Diabetic Dermopathy Detection
Early stages show faint pink discoloration only. Small patches measure just a few millimeters. You might mistake them for minor bruises initially. The color deepens gradually over weeks. Early detection signals rising blood sugar levels.
You should check your legs regularly for changes. Photograph any new marks immediately. Track their evolution carefully. Early intervention prevents additional complications. Tight glucose control slows new spot formation.
Where Does Diabetic Dermopathy Appear?
The shins represent the most common location. You will find spots on the front of the lower legs. The feet occasionally develop similar patches. Rarely, spots appear on forearms or thighs. The face almost never shows these marks.
Distribution follows areas prone to minor trauma. Poor circulation affects these regions significantly. You should examine your legs weekly. Check both sides systematically. Document any new findings promptly.
What Causes Diabetic Dermopathy?
Microvascular damage drives this skin condition. High blood sugar injures tiny blood vessels. Collagen production changes in affected areas. Minor trauma triggers spot development. Poor circulation slows healing significantly.
Nerve damage reduces sensation in the legs. You might bump your shins without noticing. The combination creates perfect conditions for spots. Genetics influences susceptibility somewhat. The duration of diabetes increases the risk substantially.
Why Understanding Diabetic Dermopathy Matters
These spots serve as visible warning signs. They indicate long-term glucose exposure damage. You should view them as motivation for better control. The presence suggests checking for other complications.
Retinopathy and neuropathy often accompany dermopathy. Early recognition prevents serious problems downstream. You gain insight into your diabetes management. Regular skin checks become essential habits. Your healthcare team appreciates this awareness.
Is Diabetic Dermopathy Dangerous?
The condition itself causes no harm whatsoever. However, it signals underlying vascular problems. You should interpret spots as diabetes markers. They indicate the need for better glucose control. The spots do not become cancerous or infected.
No treatment removes them completely. Focus on preventing new ones instead. Your doctor will monitor overall complications. The presence alone requires no emergency care.
Diabetic Dermopathy vs Necrobiosis Lipoidica
These conditions look similar but differ significantly. Necrobiosis lipoidica creates larger yellow-red plaques. The center becomes shiny and atrophic. Blood vessels show clearly through thin skin. Ulceration occurs in 30% of cases. Pain and itching affect many patients.
Dermopathy remains smaller and darker always. No ulceration develops with simple dermopathy. You need a biopsy to distinguish uncertain cases. Treatment differs dramatically between conditions.
| Feature | Diabetic Dermopathy | Necrobiosis Lipoidica |
|---|---|---|
| Size | 0.5-1 cm | 1-5 cm |
| Color | Brown | Yellow-red |
| Symptoms | None | Pain, itching |
| Ulceration | Never | Common |
| Treatment | None needed | Medical intervention |
Diabetic Dermopathy vs Stasis Dermatitis
Stasis dermatitis creates different symptoms entirely. Swelling accompanies the skin changes always. Intense itching drives patients out of control. The skin becomes thick and scaly. Brown discoloration affects larger areas.
Varicose veins appear prominently. Dermopathy remains flat and asymptomatic. No swelling occurs with simple spots. Treatment requires compression stockings for stasis. Dermopathy needs only observation, typically.
How to Treat Diabetic Dermopathy
No specific medical treatment exists for these spots. Focus your energy on glucose control instead. Maintain hemoglobin A1c below 7% consistently. Protect your legs from minor trauma. Wear long pants during outdoor activities.
Moisturize daily with fragrance-free creams. Avoid scratching or picking at spots. Regular exercise improves circulation significantly. Your doctor monitors for other complications. Patience remains your best approach.
Diabetic Dermopathy Treatment Creams and
Moisturizers keep skin healthy and supple. Look for urea-based or ceramide creams. These products prevent dryness and cracking. No prescription cream removes existing spots. Topical steroids provide no benefit here. Bleaching creams work poorly on these marks.
You should avoid harsh chemical treatments. Gentle skincare prevents additional damage. Sunscreen protects against darkening. Consistent care maintains skin integrity.
Can Diabetic Dermopathy Go Away?
Some spots fade slowly over 12-24 months. Others persist indefinitely without change. New spots may replace fading ones. Complete clearance happens rarely. You cannot predict which will disappear.
Good glucose control improves fading chances. Time remains the only true healer. Accept their presence as diabetes markers. Focus on preventing complications instead. Cosmetic concerns remain secondary to health.
How to Get Rid of Diabetic Dermopathy
Instant removal proves impossible currently. Laser therapy shows limited success only. The spots often recur after treatment. Costs outweigh benefits significantly. You should accept them as diabetes indicators.
Prevention remains more effective than removal. Tight glucose control prevents new formation. Protect legs from injury consistently. Document changes photographically. Discuss concerns with your dermatologist.
Diabetic Dermopathy on Feet and Legs
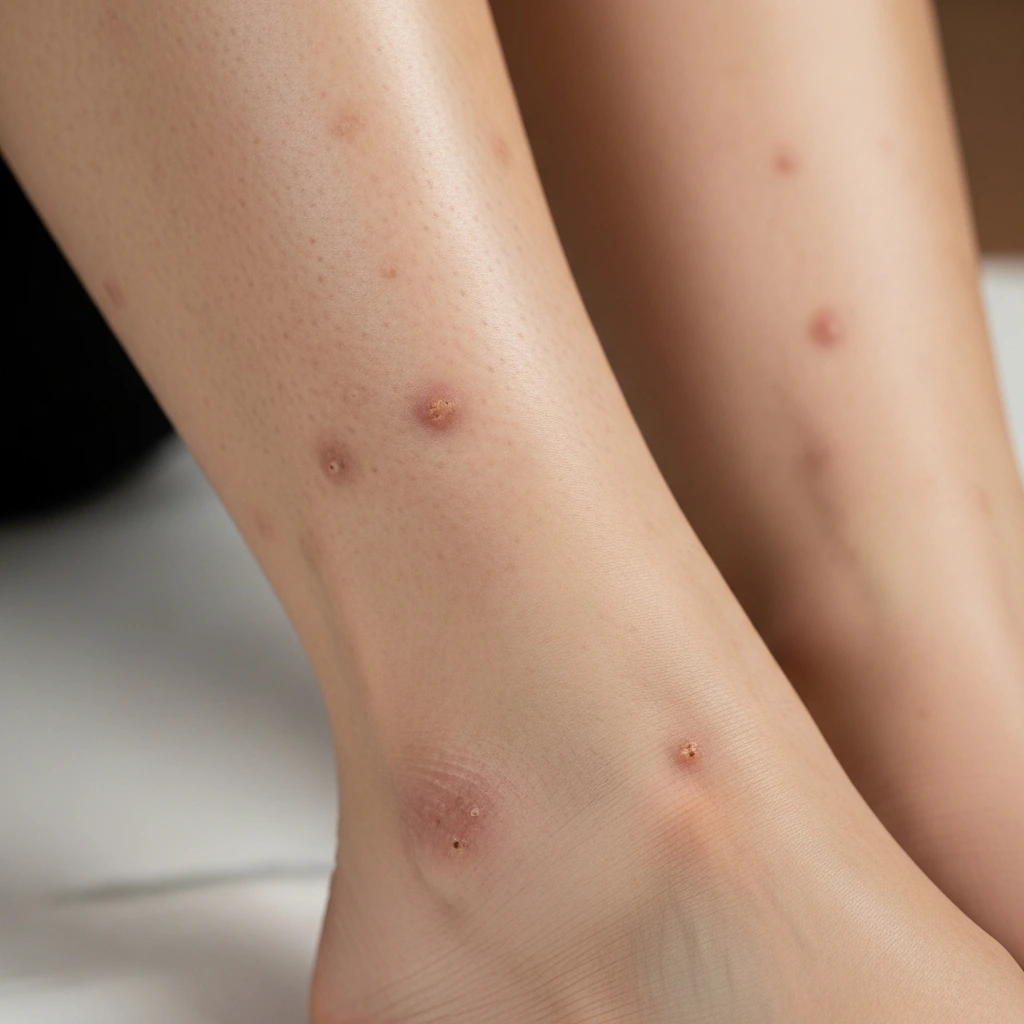
Lower extremities bear the brunt always. Poor circulation affects these areas most. You should inspect your feet daily for changes. Diabetic dermopathy on the feet requires extra attention. Combine regular checks with proper footwear.
Report any ulceration immediately to doctors. Leg elevation improves circulation somewhat. Compression stockings help venous return. Exercise strengthens calf muscles effectively. These measures support overall vascular health.
Diabetic Lower Leg Discoloration Explained
Multiple conditions cause leg discoloration in diabetes. Dermopathy creates the characteristic brown spots. Vascular changes produce generalized darkening. Hemosiderin deposition stains the skin brown. Lipodermatosclerosis creates hard, tight skin.
You need a professional diagnosis for certainty. Each condition requires different management approaches. Dermopathy remains the most benign finding. Other causes demand active treatment. Never self-diagnose leg changes.
Diabetic Skin Lesions Overview
Diabetes affects the skin through multiple mechanisms. Dermopathy represents the most common finding. Acanthosis nigricans darkens skin folds. Necrobiosis lipoidica creates serious plaques. Bullosis diabeticorum causes blister formation. Infections occur more frequently.
You should report any skin changes promptly. Early intervention prevents complications effectively. Regular dermatology visits help monitor. Skin health reflects overall diabetes control.
Diabetic Dermopathy Histology
Microscopic examination reveals specific changes. Blood vessel walls become abnormally thickened. Red blood cells leak into the surrounding tissue. Hemosiderin deposits create a brown color. Collagen bundles appear fragmented.
Epidermis thins slightly over spots. These changes confirm microvascular damage. Biopsy rarely needed for diagnosis. Clinical appearance is usually sufficient. Pathologists recognize characteristic patterns easily.
ICD-10 Code for Diabetic Dermopathy
Doctors code this as E11.628 typically. This indicates type 2 diabetes with skin complications. Type 1 diabetes uses E10.628 instead. Proper coding ensures insurance coverage. Documentation supports medical necessity.
You should understand your diagnosis codes. Accurate records help track complications. Billing requires specific code selection. Your provider handles coding appropriately.
When to See a Doctor
Rapid changes warrant immediate evaluation. Pain or tenderness develops unexpectedly. Ulceration breaks the skin’s surface. Bleeding occurs from any spot. Signs of infection appear suddenly. You notice swelling or warmth.
Multiple new spots appear quickly. Uncertain diagnosis creates anxiety. Professional evaluation provides peace of mind. Early intervention prevents serious problems.
Frequently Asked Questions
What Does Diabetic Dermopathy Look Like Initially?
Early spots appear pink or red initially. They measure just a few millimeters wide. The surface remains smooth and flat. You might mistake them for minor bruises. Color deepens to brown over weeks.
Is Diabetic Dermopathy Dangerous to My Health?
The spots themselves cause no harm. They indicate underlying blood vessel damage. You should view them as warning signs. Better glucose control prevents complications. No emergency treatment is necessary.
Can I Remove Diabetic Dermopathy Permanently?
No guaranteed removal method exists currently. Some spots fade naturally over time. Laser treatment shows inconsistent results. Focus on preventing new ones instead. Accept them as diabetes markers.
What Cream Works Best for These Spots?
No specific cream removes dermopathy effectively. Moisturizers maintain skin health generally. Urea-based products prevent dryness. Avoid harsh bleaching agents. Gentle skincare prevents additional damage.
How Quickly Do These Spots Develop?
Spots appear gradually over weeks, typically. You might notice one or two initially. More development over months or years. Good glucose control slows formation. Regular inspection catches them early.
Conclusion
In my dermatology practice, I encounter diabetic dermopathy weekly. Last month, a 58-year-old teacher showed me brown spots on her shins. She worried about skin cancer initially. After examination, I reassured her about the benign nature. We reviewed her hemoglobin A1c together—it was 8.2%.
I connected her with our diabetes educator immediately. Three months later, her A1c dropped to 6.8%. No new spots appeared. Her existing marks began fading slightly. This case illustrates why skin findings matter.
They motivate patients toward better control. I always photograph baseline lesions for comparison. Patients appreciate visual documentation of progress. We work as a team toward optimal health.

