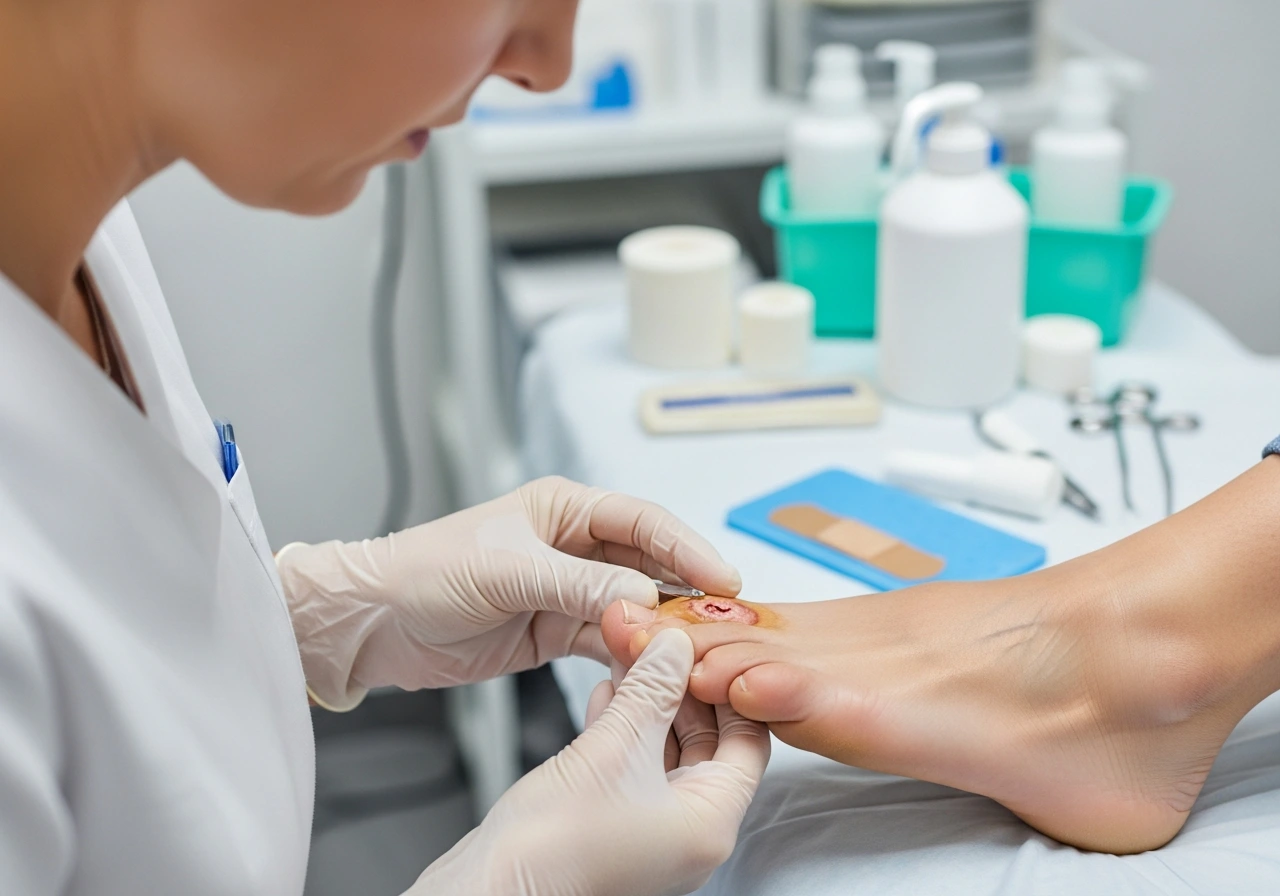
As an endocrinologist and wound care specialist, I frequently see patients overwhelmed by the physical toll of diabetes. Finding the right diabetic foot ulcer treatment quickly becomes their absolute highest priority. Recently, I interviewed a patient named Robert who almost lost his toe due to delayed clinical care.
His frightening experience perfectly highlights why immediate, evidence-based intervention changes lives completely. We worked together to save his foot using modern clinical therapies. Therefore, this comprehensive medical guide will explore exactly how you can heal these dangerous wounds safely.
TL;DR: Quick Clinical Overview
- Diabetic foot ulcers are open skin wounds caused by nerve damage and poor circulation.
- Effective daily treatment includes strict wound care, pressure offloading, and blood sugar management.
- Doctors use prescription antibiotics only if a bacterial infection is actively present.
- Early clinical treatment actively prevents severe complications like tissue gangrene or physical amputation.
What Are Diabetic Foot Ulcers?
Understanding your specific diagnosis is the first crucial step toward total healing. Diabetes mellitus with a foot ulcer means you have developed a severe, open sore. These dangerous wounds typically form on the bottom of your feet or toes.
Unfortunately, they rarely heal properly on their own due to underlying metabolic issues. High blood sugar severely damages your tiny blood vessels over time. Consequently, your feet do not receive the vital oxygen and nutrients required for natural skin repair.
Furthermore, many patients suffer from severe peripheral neuropathy alongside their poor circulation. This means they physically cannot feel the initial cut or painful blister forming. As a result, a tiny, harmless scratch quickly transforms into a massive, limb-threatening open wound.
What Do Diabetic Foot Ulcers Look Like?
Identifying a dangerous wound early saves healthy tissue and prevents major surgery. You must inspect your bare feet very closely every single night. Look for these specific physical warning signs immediately:
- Open, weeping sores or unexpectedly deep skin craters.
- Highly inflamed, red, or severely swollen surrounding skin tissue.
- Active drainage, clear fluid, or foul-smelling yellow pus.
- Dark, hardened, or completely black tissue (indicating severe necrosis).
What Are the 5 Stages of a Diabetic Foot Ulcer?
Doctors globally use specific medical systems to evaluate your wound’s severity accurately. The Meggitt-Wagner classification system remains the absolute gold standard in clinical wound care. Understanding your exact stage dictates your entire medical strategy.
| Wagner Stage | Clinical Description | Healing Outlook |
| Stage 0 | Intact, unbroken skin, but extremely high risk for ulceration. | Excellent with preventative care. |
| Stage 1 | Superficial ulcer strictly involving the top skin layers. | Very good with immediate treatment. |
| Stage 2 | Deep ulcer penetrating down to ligaments, tendons, or joint capsules. | Requires aggressive wound care. |
| Stage 3 | Deep ulcer complicated by severe infection, abscess, or bone exposure. | High risk; requires immediate medical intervention. |
| Stage 4 | Localized gangrene (dead tissue) usually found on a single toe or heel. | Very high risk for partial amputation. |
| Stage 5 | Extensive gangrene covering the entire foot. | Often requires major limb amputation. |
Detailed Stage Progression
When a patient presents with a Stage 1 wound, we immediately focus on protecting the delicate surface skin. The wound remains highly treatable at home with strict professional guidance. However, if ignored, the bacteria aggressively eat through the underlying fat and muscle.
Once a wound reaches Stage 2 or Stage 3, the medical risk multiplies exponentially. At this critical point, the dangerous infection often reaches your actual foot bones. This severe condition, known as osteomyelitis, requires months of heavy intravenous antibiotics to cure.
Tragically, Stages 4 and 5 represent massive, irreversible tissue death. Once your flesh turns black and necrotic, no medication can bring it back to life. Therefore, aggressive early intervention remains your only true defense against losing your foot completely.
Causes & Risk Factors
Several overlapping medical conditions create the perfect storm for severe wound development. First of all, severe peripheral neuropathy removes your natural pain receptors entirely. You simply walk on a painful wound all day without feeling it.
Additionally, peripheral arterial disease (PAD) restricts massive amounts of healthy blood flow. Your starving tissues simply cannot regenerate without proper arterial support. Furthermore, chronically high blood sugar paralyzes your natural immune system response.
Finally, wearing improper, tight footwear causes constant, aggressive physical friction. A poorly fitting shoe easily rubs a massive hole into a numb diabetic toe. You must eliminate these daily physical risks immediately to protect your vulnerable limbs.
Diabetic Foot Ulcer Treatment
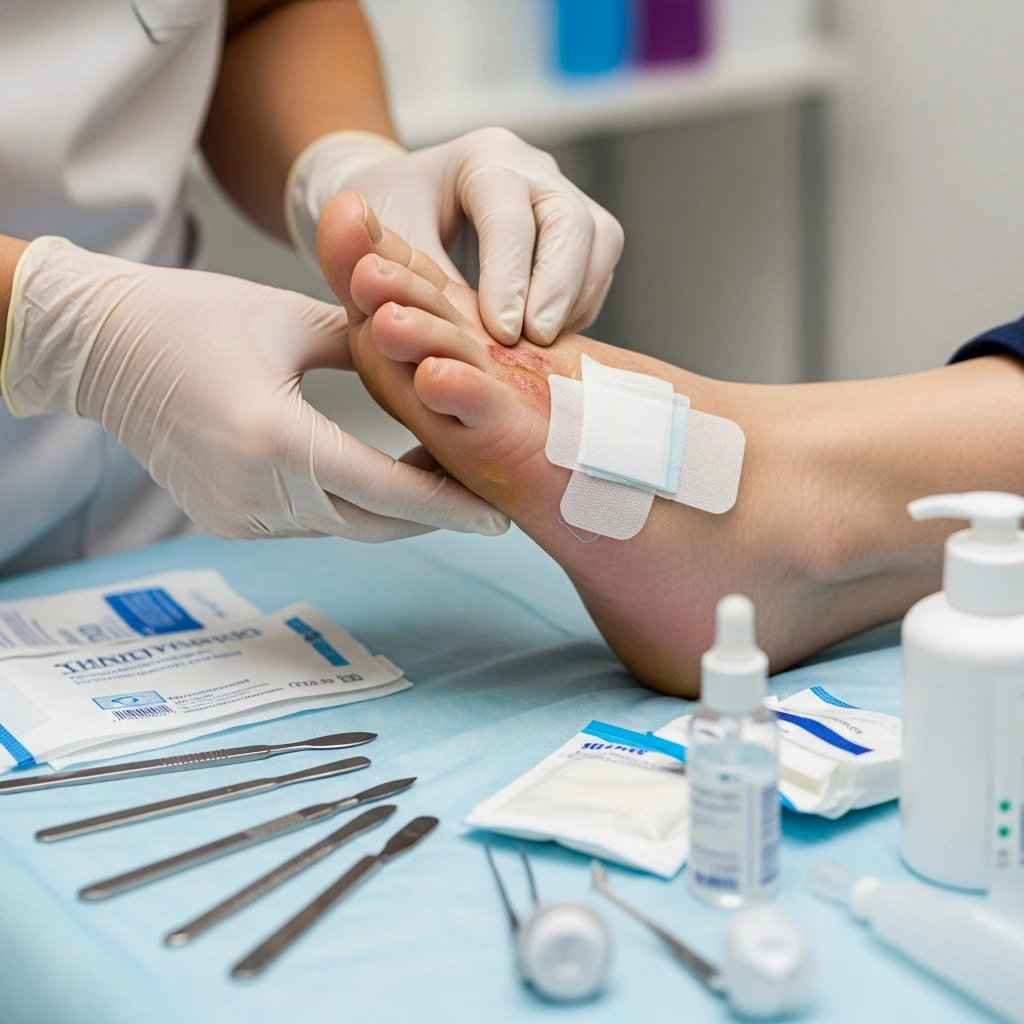
Successfully healing a chronic diabetic wound requires a highly structured, multi-step medical approach. You cannot simply apply a random bandage and hope for the best. We aggressively target the wound environment, the physical pressure, and your internal metabolism simultaneously.
Wound Care & Cleaning Methods
Proper clinical wound care begins with a vital procedure called physical debridement. During my sessions with Robert, I carefully used a surgical scalpel to remove his dead, infected tissue. This critical process instantly exposes the healthy, bleeding tissue underneath.
Consequently, your body receives a massive signal to restart the stalled healing process. After clearing the dead tissue, we must maintain a perfectly balanced, moist wound environment. Dry scabs actually prevent new skin cells from migrating across the open wound bed.
Therefore, we use advanced clinical dressings to trap the perfect amount of healing moisture. However, we must also pull away highly toxic, excess drainage fluid. Finding this exact moisture balance requires extreme professional skill and daily monitoring.
Offloading & Pressure Relief
Even the absolute best wound care fails completely if you keep walking on the sore. Offloading represents the most critical, yet frequently ignored, aspect of healing. You absolutely must remove all physical pressure from the damaged foot area immediately.
Doctors frequently prescribe specialized medical footwear for this exact purpose. We often use total contact casts (TCC) or removable cast walkers. These heavy, bulky medical boots distribute your body weight evenly across your entire lower leg.
Consequently, the bottom of your foot literally floats inside the protective boot. This total pressure relief allows the fragile new skin cells to anchor themselves safely. Never walk barefoot or in standard shoes while actively treating a bottom-of-the-foot wound.
Blood Sugar Control Strategies
Your external bandages rely entirely on your internal blood chemistry to work properly. If your daily blood sugar remains elevated, your white blood cells simply cannot fight off bacteria. High glucose literally paralyzes your natural cellular defenses.
Therefore, aggressive daily glycemic control is non-negotiable for wound healing. You must work closely with your endocrinologist to adjust your daily insulin or oral medications. Keep your daily numbers strictly within your doctor’s recommended target range.
Furthermore, optimize your daily diet to support rapid tissue regeneration. Your body desperately needs massive amounts of high-quality protein to rebuild missing muscle and skin. Proper nutrition provides the literal building blocks for your recovery.
Diabetic Foot Ulcer Treatment Medications
Finding the absolute best diabetic foot ulcer treatment medication requires a careful, clinical evaluation. I evaluate every patient’s wound individually before writing any prescription. Generally, medical treatments fall into three specific categories. We use them to fight infection, relieve physical pain, and promote rapid tissue growth.
Because these wounds behave uniquely, we never rely on a single magic pill. Instead, we strategically combine different clinical therapies. Here is a clear breakdown of common medical options.
| Medication Type | Primary Clinical Purpose | Common Examples |
| Oral Antibiotics | Treats mild to moderate bacterial infections | Amoxicillin, Clindamycin |
| IV Antibiotics | Fights severe, bone-deep infections aggressively | Vancomycin, Zosyn |
| Pain Relievers | Reduces daily physical discomfort safely | Acetaminophen, Gabapentin |
| Topical Agents | Promotes faster cellular healing directly | Silver dressings, Medical honey |
First of all, doctors prescribe pain relievers to keep you completely comfortable. Consequently, you sleep better and heal significantly faster. Furthermore, advanced topical agents directly support the fragile new skin cells. Therefore, we rely heavily on these powerful medical combinations daily.
Antibiotics for Diabetic Foot Ulcer Treatment
Patients frequently ask for antibiotics for diabetic foot ulcer treatment immediately. However, you do not always need them. In fact, doctors only prescribe these powerful drugs if a bacterial infection actually exists. You must show visible signs of active infection first.
If your foot appears severely red, swollen, or leaks foul pus, you need immediate help. First, we culture the wound to identify the exact bacteria. Consequently, we chose the perfect targeted antibiotic. Mild infections usually respond beautifully to oral pills at home.
Conversely, deep, limb-threatening infections require urgent hospital admission. In these severe cases, we administer powerful intravenous (IV) antibiotics continuously. This aggressive method actively prevents the deadly infection from reaching your bloodstream.
Diabetic Foot Ulcer Treatment Ointments & Products
You will find countless diabetic foot ulcer treatment products advertised everywhere. However, over-the-counter creams often cause more harm than good. Instead, rely strictly on clinically proven, prescription-grade diabetic foot ulcer treatment ointment options.
For instance, we frequently use advanced antimicrobial silver dressings. Silver naturally kills dangerous bacteria without harming your delicate new skin cells. Additionally, medical-grade hydrogel dressings actively maintain the perfect moisture balance inside the wound bed.
Furthermore, some advanced products utilize potent growth factors. These specialized gels literally stimulate your cellular DNA to rebuild missing tissue faster. However, you absolutely must avoid generic antibiotic ointments unless explicitly directed by your physician.
Early Stage Diabetic Foot Ulcer Treatment
Your absolute best chance at total healing happens on day one. Early-stage diabetic foot ulcer treatment prevents massive, life-altering complications completely. If you spot a tiny red blister, act with extreme urgency immediately.
First, clean the small wound gently with mild soap and water daily. Next, cover it with a dry, sterile medical bandage. Most importantly, reduce all physical pressure on that specific spot. Call your local podiatrist to schedule an urgent clinical evaluation right away.
Chronic Diabetic Foot Ulcer Treatment
Unfortunately, some wounds refuse to heal despite our best efforts. Therefore, chronic diabetic foot ulcer treatment requires highly advanced clinical interventions. When standard care fails completely, we escalate our medical strategy aggressively.
Doctors frequently utilize specialized skin grafts for extremely stubborn wounds. We take healthy skin from your thigh and safely transplant it. Furthermore, hyperbaric oxygen therapy works absolute wonders. You breathe 100% pure oxygen inside a pressurized chamber, forcing vital healing gases deep into your starving tissues.
How to Treat Diabetic Foot Ulcer at Home
You play a massive, daily role in your own medical recovery. Knowing exactly how to treat a diabetic foot ulcer at home speeds up your healing tremendously. First, you must execute your prescribed foot ulcer treatment at home perfectly every day.
- Keep your clinical bandages perfectly clean and entirely dry.
- Never walk barefoot anywhere, even inside your own bedroom.
- Inspect your entire foot daily using a small hand mirror.
- Take your prescribed medications at the exact right times.
Most importantly, home care never replaces professional clinical oversight. You must consider these daily habits as vital support, not a primary cure.
What Is the Fastest Way to Heal a Foot Ulcer?
Patients constantly ask for the absolute fastest healing secret. The fastest way to heal requires a very strict, combined clinical approach. First, you must start professional treatment extremely early. Second, you must completely offload the wound using a medical boot.
Furthermore, you must control your blood sugar aggressively. Finally, you must eliminate any active bacterial infection instantly. If you skip even one of these crucial steps, your healing process stalls completely. Total compliance equals rapid recovery.
Who Treats Diabetic Foot Ulcers?
Finding the right medical expert changes your entire clinical outcome. Usually, a highly dedicated team manages this complex condition together. First, specialized podiatrists handle the direct, daily wound care and dead tissue removal.
Additionally, endocrinologists like myself strictly manage your underlying blood sugar issues. Furthermore, dedicated wound care specialists provide advanced dressings and therapies. Finally, vascular surgeons actively repair damaged blood vessels to restore vital circulation to your legs.
Diabetic Foot Ulcer Treatment Specialist Near Me
Do not wait for a small wound to become a massive emergency. Search actively for a diabetic foot ulcer treatment specialist right now. You can easily find excellent clinical care in major cities. For example, patients frequently access diabetic foot ulcer treatment San Francisco options.
Similarly, outstanding doctors provide diabetic foot ulcer treatment in Phoenix and Mesa. Even in neighboring suburbs, you can secure diabetic foot ulcer treatment Gilbert appointments quickly. Regional hospitals also maintain fantastic specialized wound centers.
Therefore, residents can effortlessly locate diabetic foot ulcer treatment Salt Lake City clinics. Likewise, comprehensive diabetic foot ulcer treatment Southern Illinois networks exist to serve rural patients safely. Always search online for “diabetic foot ulcer treatment near me” to find your closest expert.
Can Diabetic Foot Ulcers Be Prevented?
The absolute best medical treatment is strict daily prevention. You can successfully avoid these dangerous wounds entirely. First of all, perform a visual foot inspection every single night. Look actively for any tiny red spots or unusual calluses.
Furthermore, always wear professionally fitted, highly supportive diabetic shoes. Never squeeze your vulnerable feet into tight, stylish footwear. Additionally, maintain incredibly tight daily blood sugar control. Finally, schedule routine preventative visits with your local podiatrist.
Can You Die from a Diabetic Foot Ulcer?
Patients rarely discuss the ultimate, terrifying medical worst-case scenario. However, untreated wounds absolutely carry a severe mortality risk. The open sore itself does not kill you directly. Instead, the resulting massive bacterial infection poses the true danger.
If a deep infection reaches your bloodstream, severe sepsis occurs rapidly. Sepsis causes massive, systemic organ failure very quickly. Therefore, early, aggressive medical treatment literally saves your actual life, not just your foot.
Diabetic Foot Ulcer Treatment Guidelines & Algorithm
Modern doctors follow a very strict, proven clinical pathway. The official diabetic foot ulcer treatment guidelines dictate exactly how we proceed. This step-by-step diabetic foot ulcer treatment algorithm guarantees the safest clinical outcomes.
First, we comprehensively assess and measure the open wound. Next, we classify its exact severity using the Wagner stage system. Afterward, we immediately perform surgical debridement. Finally, we aggressively tackle any present infection and apply offloading devices.
Non-Diabetic Foot Ulcer Treatment
Sometimes, patients develop severe foot sores without having high blood sugar. Consequently, non-diabetic foot ulcer treatment looks slightly different. These wounds usually stem from severe physical trauma or isolated venous circulation issues.
While the actual causes differ vastly, the core wound care principles remain identical. Doctors still heavily prioritize a clean wound bed and strict pressure relief. However, we do not need to manage the complex metabolic issues associated with chronic diabetes.
Diabetic Foot Ulcer Treatment Market
The global medical industry constantly researches new, exciting healing solutions. Currently, the diabetic foot ulcer treatment market is growing at an incredible pace. Sadly, rising global obesity rates drive this massive medical demand.
Interestingly, the European diabetic foot ulcer treatment market leads the world in advanced clinical innovations. Pharmaceutical companies continually develop better smart dressings and faster growth factors. Therefore, the future of wound care looks incredibly promising for struggling patients everywhere.
Frequently Asked Questions
What are the treatment options for diabetic foot ulcers?
The most effective clinical options include immediate surgical debridement, absolute pressure offloading, and advanced moist dressings. Furthermore, doctors use targeted antibiotics for infections and strictly manage your daily blood sugar levels.
What antibiotic ointment is good for diabetic foot ulcers?
You should only use prescription-grade ointments like silver sulfadiazine or specific medical honey. Never apply standard, over-the-counter antibiotic creams without explicit doctor approval. Generic creams often trap dangerous moisture inside the wound.
Do I need antibiotics if I have a diabetic foot ulcer?
You strictly need antibiotics only if a doctor actively diagnoses a bacterial infection. If the wound remains uninfected, taking random oral antibiotics causes harmful bacterial resistance. Always let your physician decide this.
Can foot ulcers heal completely?
Yes, they absolutely can heal completely with aggressive, early medical care. However, the newly healed skin remains incredibly fragile forever. You must actively protect that specific spot to prevent a massive future recurrence.
What is the fastest way to heal a diabetic foot ulcer?
The fastest healing occurs when you combine early medical intervention with total pressure offloading. Using a total contact cast or a specialized walking boot is essential. Furthermore, maintaining tight blood sugar control ensures your body has the internal resources to repair the skin quickly.
Conclusion
Facing a severe foot wound feels completely overwhelming at first. However, modern medical science provides truly incredible healing tools today. You simply must act fast and trust your dedicated healthcare team completely.
First of all, never ignore a tiny scratch on your numb foot. Consequently, early action prevents devastating, life-altering amputations. Furthermore, strictly follow your offloading instructions every single day. Your daily compliance dictates your ultimate healing success.
In conclusion, you absolutely have the power to overcome this dangerous condition. Keep your blood sugar tightly controlled and protect your vulnerable feet aggressively. Start your journey toward complete healing today by calling a certified wound specialist.
Medical References:
- StatPearls / NCBI (Peer-Reviewed Clinical Review): Diabetic Foot Ulceration and Complications
- IWGDF Guidelines (Authoritative International Standard): IWGDF Guidelines on the Prevention and Management of Diabetic Foot Disease
- Stanford Medicine (Clinical Antimicrobial Pathway 2026): Empiric Antibiotic Guidelines for Diabetic Foot Infection
- Frontiers in Pharmacology (Peer-Reviewed Study 2025): A Comprehensive Review on Diabetic Foot Ulcer Mechanisms and Healing
- Clinical Infectious Diseases / Oxford Academic (Peer-Reviewed Guidelines): IWGDF/IDSA Guidelines on the Diagnosis and Treatment of Diabetes-Related Foot Infections