Have you ever felt suddenly shaky, dizzy, or extremely hungry even though you recently ate? For many people, these uncomfortable moments may be linked to low blood sugar, a condition medically known as Hypoglycemia. Understanding the causes of hypoglycemia is important because this condition can happen when the body’s blood sugar drops too low for normal function.
The causes of hypoglycemia may include skipping meals, taking too much insulin or diabetes medication, intense physical activity, drinking alcohol without enough food, or certain medical conditions that affect how the body regulates glucose.
Understanding the causes of hypoglycemia is essential because this condition can affect both people living with diabetes and those without it. In simple terms, the causes of hypoglycemia are the factors that lower blood glucose below the normal range.
This can happen when someone takes too much insulin or diabetes medication, skips meals, exercises intensely, or drinks alcohol without eating enough food. However, low blood sugar is not limited to diabetes alone. Certain illnesses, hormonal imbalances, or even prolonged fasting can also trigger it.
Because the brain relies heavily on glucose for energy, recognizing the causes of hypoglycemia early is important for preventing confusion, weakness, fainting, and other serious complications. In this guide, we’ll explore what Causes low blood sugar without diabetes and what both diabetics and non-diabetics should know.
TL;DR: The Main Causes of Hypoglycemia
If you or a loved one is experiencing sudden, terrifying energy crashes, here is the quick medical bottom line:
- The Core Definition: Hypoglycemia occurs when your blood sugar drops dangerously low, typically below 70 mg/dL. Consequently, your brain and body are literally starving for essential energy.
- Common Diabetic Causes: For people managing diabetes, the most frequent triggers are accidental insulin overdoses, skipping meals after taking medication, or engaging in intense, unplanned exercise.
- Non-Diabetic Triggers: You do not need diabetes to experience a crash. First of all, heavy binge drinking on an empty stomach completely stalls your liver’s normal glucose production. Furthermore, severe liver disease, kidney failure, and rare hormone disorders are massive underlying culprits.
- Dangerous Warning Signs: Initially, you will feel extremely shaky, sweaty, and intensely hungry. However, if your blood sugar falls below 40 mg/dL, you face a life-threatening risk of seizures, coma, and neuroglycopenic shock.
What Is Hypoglycemia?
Before diving into the triggers, we must clearly define the condition. Hypoglycemia simply means your blood glucose (sugar) is dangerously lower than what your body needs to function. Glucose is your brain and body’s primary energy source. When this energy source plummets, your body immediately triggers a fight-or-flight response.
You might experience a rapid heartbeat, cold sweats, intense hunger, and severe anxiety. Many patients ask, ” Is hypoglycemia diabetes?” The straightforward answer is no. While it is a very frequent complication of diabetes management, hypoglycemia itself is a distinct physiological state that can happen to anyone.
Common Causes of Hypoglycemia
To properly manage your health, you must identify the common causes of hypoglycemia. Your body relies on a delicate balance between the food you eat, the hormones you produce, and the energy you burn. When this balance breaks down, blood sugar drops rapidly.
The most common cause of hypoglycemia is undoubtedly related to diabetes medications, specifically insulin overadministration. However, several other everyday factors are major triggers. Skipping meals or fasting dramatically reduces your circulating glucose.
If you take medications but forget to eat, your blood sugar has nowhere to go but down. Additionally, consuming excessive alcohol heavily disrupts your liver’s normal functions. Your liver normally releases stored glucose into your bloodstream when you need energy.
However, when processing alcohol, the liver stops this glucose release, leading to rapid drops. Finally, intense, unplanned exercise rapidly drains your muscle’s glucose reserves, causing severe post-workout crashes.
Causes of Hypoglycemia in People With Diabetes
For individuals managing a metabolic illness, the causes of hypoglycemia in diabetics usually stem from overtreatment. Managing low or high blood sugar requires perfectly matching your medication dosage with your food intake and physical activity.

If a patient injects too much rapid-acting insulin before a meal, their blood sugar will plummet. Similarly, taking certain oral medications, like sulfonylureas, forces the pancreas to pump out excess insulin regardless of what you eat. If you delay a meal after taking these drugs, you will experience a severe hypoglycemic event. So you should eat best breakfast at the perfect time after taking the drugs.
Which Type of Diabetes Causes Hypoglycemia?
Many newly diagnosed patients wonder which type of diabetes causes hypoglycemia. Technically, both main types can lead to low blood sugar, but the frequency and underlying reasons differ significantly based on the treatment plan. The causes of hypoglycemia in type 1 diabetes are highly prevalent because these patients produce zero natural insulin.
They rely entirely on synthetic insulin injections or pumps, making accidental overdoses much more common. Conversely, type 2 diabetics usually only experience severe lows if they are prescribed insulin therapy or specific insulin-stimulating oral medications.
Causes of Hypoglycemia Without Diabetes
While less common, the causes of hypoglycemia without diabetes are critical to understand. Doctors refer to this as non-diabetic hypoglycemia, and it requires extensive medical testing to uncover the hidden root issue. First, severe hormone deficiencies can disrupt glucose production.
If your adrenal or pituitary glands fail to produce hormones like cortisol or growth hormone, your body struggles to maintain normal blood sugar. Furthermore, severe liver diseases, such as advanced cirrhosis or hepatitis, physically destroy the liver’s ability to store and release glucose properly.
Another primary factor involves non-diabetic medications. Certain drugs, including quinine (used for malaria) and certain beta-blockers, can accidentally trigger low blood sugar. Finally, a rare pancreatic tumor called an insulinoma can secrete massive, uncontrollable amounts of insulin into the bloodstream. This constantly drives blood sugar down, regardless of how much the patient eats.
Reactive Hypoglycemia
Sometimes, the timing of your symptoms gives doctors the biggest clue. Reactive hypoglycemia specifically refers to a drastic blood sugar drop that occurs within a few hours after eating a heavy meal. This condition often happens when the body dramatically overreacts to high-carbohydrate foods, producing far too much insulin in response.
Consequently, this massive insulin spike clears out the glucose too quickly, leaving you exhausted and shaky. It is also a very common side effect for patients who have undergone gastric bypass surgery, as their modified digestive tract processes food unusually fast.
Causes of Hypoglycemia in Children
When exploring the causes of hypoglycemia in children, the clinical approach changes entirely. Children naturally have much smaller livers and less muscle mass than adults. Consequently, their bodies simply cannot store massive amounts of reserve glucose for emergencies.
A simple stomach bug that causes vomiting and diarrhea can rapidly deplete a toddler’s glucose stores. Because they cannot keep food down, their blood sugar drops dangerously fast. Fasting for prolonged periods, especially during acute illnesses, is a massive pediatric trigger.
Furthermore, some children are born with rare genetic metabolic disorders. Conditions like glycogen storage disease physically prevent a child’s liver from converting stored glycogen back into usable glucose. If left undiagnosed, these children suffer severe, chronic low blood sugar episodes.
Causes of Hypoglycemia in Newborns
The neonatal period carries extremely unique risks. If you are a new parent, understanding the causes of hypoglycemia in newborns is vital for your baby’s brain development. During pregnancy, the baby relies entirely on the mother’s glucose supply through the umbilical cord.
People frequently ask, “What are 4 common causes of newborn hypoglycemia?” First, maternal diabetes is the leading cause; if the mother’s sugar is high, the baby produces excess insulin, which causes a crash right after birth. Second, premature birth leaves babies without adequate glycogen reserves.
Third, severe neonatal infections (sepsis) rapidly burn through the infant’s available energy stores. Finally, blood type incompatibilities between the mother and baby can severely stress the infant’s metabolic system, dropping their glucose levels rapidly. Immediate feeding or IV glucose is strictly required to prevent brain injury.
Causes of Hypoglycemia in Adults
Aside from diabetes medications, the causes of hypoglycemia in adults frequently point toward hidden organ dysfunction. As we age, our internal organs slowly lose their metabolic efficiency. When major organs begin failing, blood sugar regulation completely collapses.
For instance, severe kidney failure drastically alters how insulin is cleared from the bloodstream. If the kidneys cannot filter properly, insulin circulates much longer than normal, driving blood sugar down dangerously. Similarly, advanced liver disease prevents the vital storage of backup glucose.
Additionally, non-diabetic adults who engage in heavy binge drinking on an empty stomach face immediate risks. Alcohol acts as a massive metabolic block in the liver. It forces the liver to process the toxins instead of releasing life-saving glucose into the bloodstream.
Causes of Hypoglycemia in Dogs and Cats
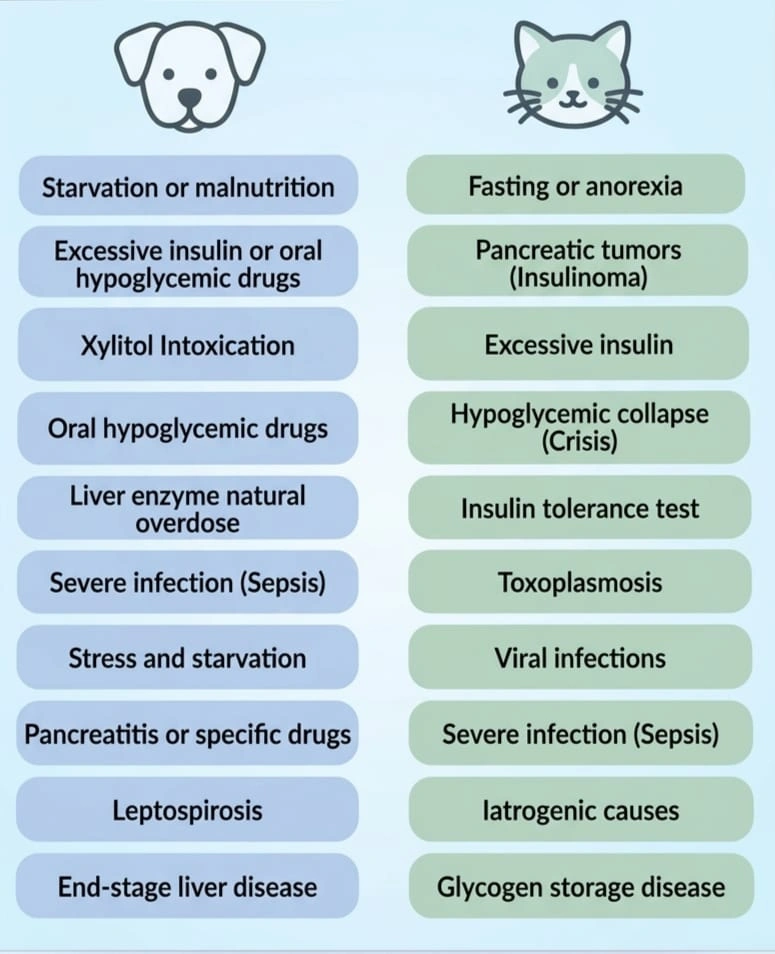
Interestingly, low blood sugar is a massive veterinary emergency as well. The causes of hypoglycemia in dogs often mirror human issues, particularly in diabetic pets. If an owner accidentally administers an insulin overdose, the dog’s blood sugar will plummet rapidly, causing severe lethargy or seizures.
However, a very specific and deadly cause of hypoglycemia in dogs involves xylitol toxicity. Xylitol is a common artificial sweetener found in sugar-free gum and peanut butter. When a dog eats it, its pancreas mistakenly releases a massive, lethal surge of insulin.
Similarly, the causes of hypoglycemia in cats often involve severe liver disease or overwhelming bacterial infections. Furthermore, very young toy dog breeds (like Chihuahuas) frequently suffer from low blood sugar simply because they lack the physical muscle mass to store enough glucose between meals.
Hypoglycemia Unawareness
One of the most terrifying clinical phenomena I analyze in patient data is hypoglycemia unawareness. The causes of hypoglycemia unawareness are deeply tied to severe, long-term nerve damage. Normally, a dropping blood sugar level triggers the brain to release adrenaline, causing the classic shaking and sweating.
However, if a patient experiences frequent, repeated low blood sugar episodes over many years, their brain literally stops sending out the adrenaline warning signal. The nervous system becomes completely desensitized to the danger.
Consequently, these patients feel absolutely fine until their blood sugar drops so low that they suddenly collapse or lose consciousness. Reversing this dangerous unawareness requires strictly avoiding any low blood sugar episodes for several weeks to let the brain’s alarm system reset.
What Level of Hypoglycemia Is Dangerous?
Understanding your lab numbers is the absolute best way to stay safe. Patients frequently ask, ” What level of low blood sugar is dangerous? In the medical community, a reading below 70 mg/dL is the official threshold for a hypoglycemic event.
However, symptoms become highly critical as the numbers drop further. If you are wondering what level of hypoglycemia causes seizures, the risk skyrockets when blood sugar falls below 40 mg/dL. At this profound stage, your brain is entirely starving for energy.
Here is a quick clinical reference for blood sugar severity:
- 70 mg/dL to 55 mg/dL: Mild hypoglycemia (shaking, sweating, hunger).
- 54 mg/dL to 40 mg/dL: Clinically significant (confusion, blurred vision, extreme weakness).
- Below 40 mg/dL: Severe hypoglycemia (seizures, loss of consciousness, coma).
Can hypoglycemia cause shock?
When blood sugar drops into those severe ranges, the body’s systems begin shutting down. Many nursing students and caregivers ask, What type of shock does profound hypoglycemia cause? The medical term for this exact emergency is neuroglycopenic shock.
Because the human brain absolutely requires a constant stream of glucose to survive, starving it causes catastrophic neurological failure. Hypoglycemia causes a type of shock, which is explained by looking at the brain’s inability to maintain basic life functions, leading to massive blood pressure drops and a comatose state.
Unlike hypovolemic shock (caused by blood loss), neuroglycopenic shock is strictly driven by an energy deficit. Administering an emergency glucagon injection or intravenous dextrose is the only way to reverse this specific type of shock before permanent brain damage occurs.
Why Am I Suddenly Getting Hypoglycemia?
If you have never had metabolic issues before, you might be desperately searching, “Why am I suddenly getting hypoglycemia?” A sudden onset in an otherwise healthy adult is a major clinical red flag that demands immediate medical testing.
First of all, have you recently changed your diet? Jumping into extreme, restrictive fasting or a strict ketogenic diet can cause severe transitional blood sugar crashes. Second, examine your medicine cabinet. Starting a new prescription, like certain antibiotics or blood pressure medications, can inadvertently trigger unexpected drops.
Finally, a sudden onset could indicate an emerging endocrine disorder. Your thyroid or adrenal glands might be struggling to produce the hormones necessary for glucose balance. Never ignore a sudden change in your body’s energy regulation; consult a doctor immediately.
What Conditions Mimic Hypoglycemia?
Because the symptoms of low blood sugar—sweating, rapid heartbeat, and shaking—are driven by adrenaline, they are not entirely unique. Therefore, doctors must often determine what mimics hypoglycemia to avoid misdiagnosis.
A severe panic or anxiety attack is the most common mimic. During a panic attack, your body dumps massive amounts of adrenaline into your bloodstream, causing exactly the same shaky, terrifying physical sensations, even though your blood sugar is perfectly normal.
Additionally, severe dehydration and a heart condition called Postural Orthostatic Tachycardia Syndrome (POTS) can cause profound dizziness and weakness when standing up. To confirm true hypoglycemia, you must physically test your blood sugar with a monitor during the episode.
Is hypoglycemia dangerous?
To summarize, the absolute gravity of this condition, is hypoglycemia dangerous? Yes, it is a medical emergency. While mild episodes can be quickly fixed with a glass of juice, ignoring the root causes invites disaster. Life-threatening hypoglycemia occurs when the brain is deprived of glucose for too long.
This can result in massive, irreversible brain damage or a fatal coma. Furthermore, experiencing a sudden low while driving a vehicle or operating heavy machinery frequently leads to tragic accidents. You must treat every single low blood sugar reading with deep clinical respect. Always carry fast-acting glucose tablets or gel, and work closely with your medical team to adjust the underlying triggers.
Frequently Asked Questions
What are the causes of hypoglycemia?
The primary triggers include overdosing on diabetes medications, skipping meals, heavy alcohol consumption without food, and intense, unplanned exercise. Rare tumors and severe organ failure can also cause it.
What causes low blood sugar without diabetes?
In non-diabetics, it is often triggered by heavy binge drinking, certain non-diabetic medications (like quinine), severe liver or kidney disease, and rare hormone deficiencies. Gastric bypass surgery can also trigger reactive lows.
What level of hypoglycemia is dangerous?
Any reading below 70 mg/dL requires immediate treatment. However, dropping below 54 mg/dL is clinically significant, and falling below 40 mg/dL is highly dangerous, risking seizures and coma.
Is hypoglycemia dangerous?
Absolutely. Severe, untreated low blood sugar starves the brain of vital energy, which can quickly lead to unconsciousness, irreversible neurological damage, and, in extreme cases, death.
What are 4 common causes of newborn hypoglycemia?
The four most frequent triggers in newborns are maternal diabetes during pregnancy, premature birth, severe neonatal infections, and blood type incompatibilities between the mother and the infant.
Conclusion
Ultimately, understanding the true causes of hypoglycemia is your most powerful tool for preventing a dangerous medical emergency. Whether you are managing chronic diabetes or experiencing strange, sudden energy crashes, your body is sending you a very clear physiological signal.
First of all, you must always listen to those vital early warning signs like shaking, sudden sweating, and intense hunger. Furthermore, keeping a detailed daily log of when your blood sugar drops provides essential clinical clues for your doctor.
For instance, carefully tracking your medication timing, exercise habits, and meals can quickly pinpoint your exact trigger. Consequently, this simple tracking habit allows your medical team to safely adjust your insulin or investigate hidden, non-diabetic metabolic issues.
Most importantly, never try to diagnose severe, recurring hypoglycemia completely on your own. Because life-threatening blood sugar drops can happen so rapidly, you must consult a qualified healthcare provider for proper diagnostic testing. Finally, always be proactive by keeping fast-acting glucose tablets or a small box of juice nearby, no matter where you go.
Evidence-Based References:
- Centers for Disease Control and Prevention (CDC) – Low Blood Sugar (Hypoglycemia)
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK)
- American Diabetes Association (ADA) – Hypoglycemia
- Mayo Clinic – Hypoglycemia Symptoms and Causes
- Cleveland Clinic – Hypoglycemia (Low Blood Sugar)

