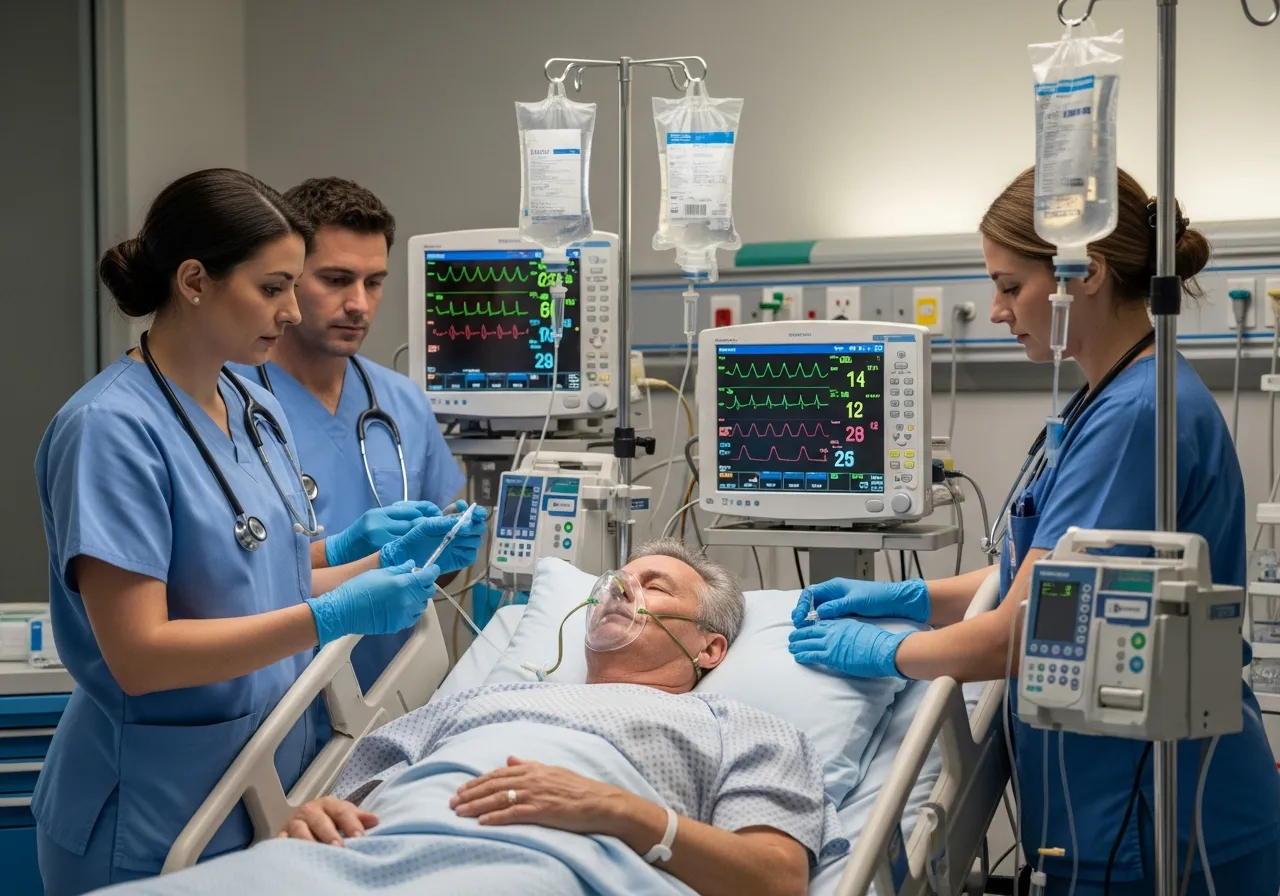
Dealing with a diagnosis of diabetes is often a massive life shift. However, nothing is quite as scary as facing a sudden metabolic crisis. Have you ever felt that strange, fruity scent on your breath or noticed your heart racing for no clear reason? These can be the first signs of a dangerous complication.
Getting the right diabetic ketoacidosis treatment quickly is truly a matter of life or death. As a physician, I have sat at many bedsides in the ICU watching patients fight through this. I once interviewed a young patient named Sarah who didn’t realize her insulin pump had failed.
She thought she just had the flu. By the time she reached us, her body was dangerously acidic. Her story is a vital reminder of why we must act fast.
In this guide, we will break down exactly how doctors manage this condition. We will look at hospital protocols and the latest 2025 guidelines. Most importantly, you will learn how to spot the warning signs before they become a crisis.
Key Takeaways for Your Safety
- Act Fast: DKA is a life-threatening emergency.
- Hospital is Best: You need IV fluids and expert monitoring.
- Know the Signs: Fruity breath, vomiting, and confusion are red flags.
- Prevention: Never skip insulin doses, especially when you are sick.
What Is Diabetic Ketoacidosis?
Diabetic ketoacidosis is a severe, life-threatening complication of diabetes. It happens when your body does not have enough insulin to use sugar for energy. Instead, it starts burning fat at a dangerously fast rate.
This process produces a buildup of acids in the bloodstream called ketones. If these ketones stay high, they turn your blood acidic. This state is known as metabolic acidosis. Without a proper diabetic ketoacidosis treatment plan, your organs can begin to fail very quickly.
While it is most common in people with Type 1 diabetes, those with Type 2 can also develop it. This usually happens during times of extreme physical stress or severe infection.
DKA Criteria and Diagnosis
Doctors use very specific “benchmarks” to diagnose this condition. When you arrive at the hospital, the medical team will run several blood tests immediately.
The primary DKA criteria include:
- Blood Glucose: Usually higher than 250 mg/dL.
- Blood pH: A level lower than 7.3 (indicating acidity).
- Bicarbonate Level: Typically lower than 18 mEq/L.
- Ketones: High levels of beta-hydroxybutyrate, DKA markers in the blood or urine.
Measuring beta-hydroxybutyrate is often more accurate than simple urine strips. It shows the real-time status of your blood chemistry. This helps us tailor the diabetic ketoacidosis treatment to your specific needs.
What Causes Ketoacidosis?
Understanding what causes ketoacidosis is the first step in prevention. In my clinical experience, most cases stem from a few common triggers.
First, missed insulin doses are a frequent culprit. This might happen due to a pump malfunction or a forgotten injection. Second, illness or infection can trigger the body to produce “stress hormones.”
These hormones, like adrenaline and cortisol, actually block the effects of insulin. This is why you might see high ketones even if you haven’t changed your diet.
Finally, certain medications can cause issues. For instance, SGLT2 inhibitors can lead to a rare version of this condition where blood sugar looks normal. Always tell your doctor about every medication you take.
Diabetic Ketoacidosis Risk Factors
Who is most at risk? While anyone with diabetes can face this, certain factors make it more likely.
Diabetic ketoacidosis risk factors include:
- Having Type 1 diabetes.
- Being under the age of 19.
- Recent physical trauma or surgery.
- High levels of emotional stress.
- Frequent “brittle” blood sugar swings.
In many cases, DKA is actually the first sign that a person has diabetes. This is especially true in children. If you notice extreme thirst and frequent urination, do not wait to get tested.
What Type of Treatment Does DKA Require?
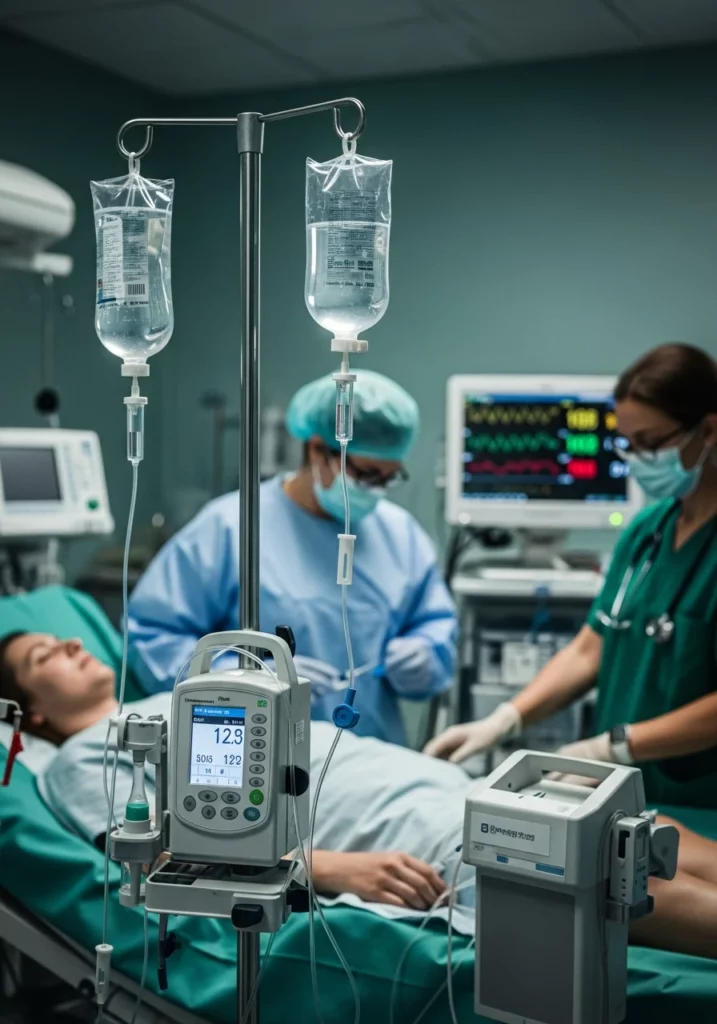
You might wonder what type of treatment diabetic ketoacidosis requires specifically. Because the body is in a state of chemical chaos, the treatment must be multi-layered.
There are three pillars of care:
- Fluid Resuscitation: This fixes dehydration and dilutes excess sugar.
- Insulin Therapy: This stops the body from breaking down fat into ketones.
- Electrolyte Replacement: This prevents heart rhythm problems.
Each of these must be balanced carefully by a medical team. If we give insulin too fast without enough fluids, your blood pressure could drop. It is a delicate medical “dance” that requires constant monitoring.
Diabetic Ketoacidosis Treatment Protocol
The diabetic ketoacidosis treatment protocol is a step-by-step map doctors follow. It ensures that the most dangerous issues are handled first.
- Hour 1: We start high-volume IV saline fluids. We also check potassium levels immediately.
- Hour 2 and Beyond: We begin a continuous insulin drip. We check your blood sugar every single hour.
- Ongoing: We monitor “anion gap” and pH levels. This tells us when the blood is finally becoming less acidic.
This diabetic ketoacidosis treatment algorithm is designed to be slow and steady. Moving too quickly can cause the brain to swell, which is a major risk in younger patients.
Diabetic Ketoacidosis Treatment Guidelines
Medical professionals rely on diabetic ketoacidosis treatment guidelines to provide the best care. Organizations like the American Diabetes Association (ADA) update these often.
The diabetic ketoacidosis treatment guidelines 2025 emphasize “patient-centered” care. This means we look at your kidney function and heart health before choosing fluid types.
Modern guidelines also suggest using “balanced” fluids instead of just plain saline. This can help clear the acid from your blood even faster. These diabetic ketoacidosis treatment guidelines, ADA experts provide, ensure that whether you are in New York or London, you receive the gold standard of care.
Diabetic Ketoacidosis Treatment in Hospital
Almost all cases of diabetic ketoacidosis treatment in hospital settings occur in the ICU or a Step-Down unit. You will likely be hooked up to several IV lines.
Expect to have your blood drawn very frequently—often every two hours. This is necessary to track your electrolytes. We specifically look at potassium, magnesium, and phosphate.
The nursing staff will also monitor your “ins and outs.” This means they track how much fluid you drink and how much you urinate. It feels intense, but this level of detail is what keeps you safe.
Insulin Therapy in DKA
The most critical part of the process is diabetic ketoacidosis treatment, insulin therapy. However, we don’t just give a standard shot under the skin.
Instead, we use an IV insulin drip. This allows the medicine to go directly into your bloodstream. It works instantly and can be adjusted minute-by-minute.
The goal isn’t just to lower blood sugar. The real goal is to “turn off” the production of ketones. We often keep the insulin drip going even after your blood sugar looks normal, just to make sure the acid is completely gone.
Can You Treat DKA at Home?
I often get asked: Can you get out of DKA at home? The answer is a very firm no. Diabetic ketoacidosis treatment at home is impossible and dangerous.
While you can treat mild “ketosis” with water and extra insulin, once you reach “acidosis,” you need IV minerals. You cannot drink enough water to fix the severe dehydration DKA causes.
Furthermore, your potassium levels can swing wildly. This can cause your heart to stop without warning. If your ketone meter reads “High” or “Large,” put down the water glass and head to the emergency room.
Euglycemic Diabetic Ketoacidosis Treatment
A tricky version of this condition is euglycemic diabetic ketoacidosis treatment. In this case, the patient has all the acid buildup, but their blood sugar is under 250 mg/dL.
This often happens to people taking SGLT2 inhibitor medications (like Jardiance or Farxiga). Because the sugar looks “normal,” people often delay going to the hospital.
The treatment is similar to standard DKA, but we give IV glucose (sugar) along with the insulin. This allows us to give enough insulin to stop the ketones without making the blood sugar drop too low.
Non-Diabetic Ketoacidosis Treatment
Did you know you can have ketones without having diabetes? This is called non diabetic ketoacidosis treatment.
This usually happens due to:
- Extreme starvation or “crash” dieting.
- Chronic alcoholism (Alcoholic Ketoacidosis).
- Prolonged, severe vomiting.
The main difference here is that the body usually needs sugar and fluids, not necessarily insulin. In these cases, the pancreas still works, but the body has run out of its stored fuel.
Diabetic Ketoacidosis Treatment in Children
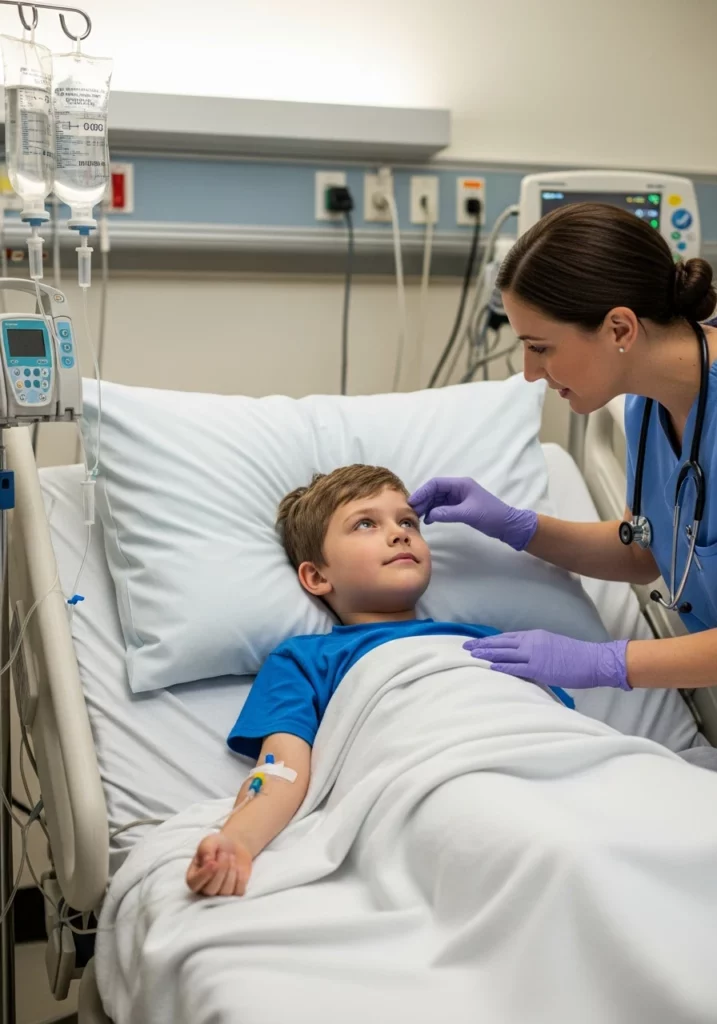
Treating kids requires an even higher level of caution. Diabetic ketoacidosis treatment in children is different because their brains are more sensitive to fluid shifts.
Pediatric protocols involve very slow fluid replacement. We use a “two-bag” system to precisely balance the sugar and electrolytes.
The biggest fear in children is cerebral edema, or brain swelling. Doctors will check a child’s neurological status every hour. They will look for signs like headaches or sudden sleepiness.
DKA Complications
Even with the best diabetic ketoacidosis treatment methods, complications can occur. It is important to know what we are watching for in the hospital.
Common DKA complications include:
- Hypokalemia: Dangerously low potassium levels.
- Cerebral Edema: Swelling of the brain.
- Acute Kidney Injury: Temporary damage to the kidneys from dehydration.
- Hypoglycemia: Blood sugar drops too low during insulin therapy.
Most of these are avoidable if the medical team monitors you closely and adjusts your IVs regularly.
Can You Die from Diabetic Ketoacidosis?
It is a heavy question, but patients need to know: Can you die from diabetic ketoacidosis? Unfortunately, yes. Before the discovery of insulin, DKA was almost 100% fatal.
Today, the mortality rate is less than 1% in specialized centers. However, this depends entirely on how fast you get help.
If treatment is delayed, the acid eventually shuts down the heart and brain. This is why “sick day rules” are so important for every person with diabetes to learn.
How Long Does It Take to Recover from DKA?
Most patients ask: How long does it take to recover from diabetic ketoacidosis? Generally, you will stay in the hospital for 24 to 72 hours.
The “acute” phase usually clears within 24 hours. This is when your blood pH returns to normal, and you can start eating again.
However, you might feel exhausted for a week or more. Your body has been through a metabolic “marathon.” It takes time for your muscles and brain to feel 100% again.
Can Someone Recover from Ketoacidosis?
The good news is that you absolutely can help someone recover from ketoacidosis and live a long, healthy life. It does not mean your diabetes is “worse” forever.
Recovery involves a “post-game” analysis. We look at why it happened. Was it a clogged pump site? Was it a silent urinary tract infection?
Once we find the trigger, we create a plan to prevent it from happening again. Most patients leave the hospital with a renewed focus on their health.
Diabetic Ketoacidosis Treatment Methods Overview
To summarize, the management of diabetic ketoacidosis is a clinical balancing act. We use specific tools to restore your health.
| Treatment Method | Purpose |
| Isotonic Fluids | Restores blood volume and kidney flow. |
| Potassium Chloride | Prevents dangerous heart arrhythmias. |
| IV Regular Insulin | Stops ketone production and lowers sugar. |
| Bicarbonate | Only used in extreme cases to fix pH. |
These diabetic ketoacidosis treatment methods are the pillars of modern emergency endocrinology.
Treatment Goals in DKA
What is the doctor’s “finish line”? The diabetic ketoacidosis treatment goals are very clear in our medical charts.
We want to see:
- A blood pH level above 7.3.
- An anion gap lower than 12.
- A patient who can eat and drink without vomiting.
- A stable transition back to “under-the-skin” insulin injections.
Once these goals are met, you are usually safe to go home.
Special Cases: DKA in Dogs
Believe it or not, our furry friends can get this, too. Diabetic ketoacidosis treatment in dogs is very similar to human care.
If your dog is acting lethargic, vomiting, or has “sweet” breath, get them to a vet. They will also need IV fluids and specialized animal insulin to recover. It is just as much of an emergency for them as it is for us.
Diabetic Ketoacidosis Treatment Market Overview
The diabetic ketoacidosis treatment market is growing. This is sadly due to the rising rates of diabetes worldwide.
We are seeing a massive shift toward better monitoring tools. New “smart” insulin pumps and continuous ketone monitors (CKMs) are the future. These tools help patients catch rising ketones hours before they become a medical emergency.
Action Plan: What to Do If You Suspect DKA
- Test Immediately: Check your blood sugar and blood ketones right away.
- Call for Help: If ketones are “Moderate” or “High,” call your doctor or 911.
- Do Not Exercise: Exercise can actually make ketones rise faster if your insulin is low.
- Head to the ER: If you are vomiting and cannot keep fluids down, you must go to the hospital.
Frequently Asked Questions (FAQs)
What is the best treatment for diabetic ketoacidosis?
The gold standard is a combination of IV saline for hydration, IV insulin to stop ketone production, and potassium to protect the heart. This must be done in a hospital.
Can DKA be treated at home?
No. While you can manage very mild ketones with a doctor’s guidance, true DKA involves blood acid changes that require hospital-grade IV minerals and monitoring.
How serious is DKA?
It is extremely serious. Without medical intervention, DKA leads to coma and death. However, with prompt hospital care, most people recover fully.
How long does recovery take?
The hospital stay is usually 1 to 3 days. Most people feel back to their “normal” self within a week, provided they follow their follow-up care plan.
Does DKA only happen in Type 1 diabetes?
No. While more common in Type 1, people with Type 2 diabetes can develop DKA during severe infections, heart attacks, or while taking certain medications like SGLT2 inhibitors.
Conclusion: Navigating the Path to Recovery
In summary, facing a metabolic crisis is a major life event. It requires quick thinking and even faster medical action. However, the modern medical system is well-equipped to handle this challenge.
With the right hospital care, you can bounce back stronger than before. You will have a better understanding of your insulin needs. You will also know how to spot the early warning signs. This knowledge is your most powerful tool for long-term health.
Always remember that time is the most critical factor. If you feel the symptoms, do not hesitate to seek help. Professional diabetic ketoacidosis treatment is the only safe way to restore your health and protect your future.
Medical References:
- PubMed (Clinical Review): Management of Diabetic Ketoacidosis (2023)
- National Institutes of Health (NIH) StatPearls: Adult Diabetic Ketoacidosis Management Protocols
- American Diabetes Association (ADA): Standards of Care in Diabetes (2024/2025)
- Centers for Disease Control and Prevention (CDC): Diabetes-Related Ketoacidosis Public Health Guidance
- Mayo Clinic: Diabetic Ketoacidosis: Diagnosis and Emergency Treatment