Managing diabetes can often feel like a relentless, overwhelming full-time job, especially when your treatment relies heavily on multiple daily injections. What is an insulin pump? This question is crucial for many patients who find themselves grappling with constant math, needle fatigue, and unpredictable blood sugar swings, leaving them searching for a better, more stable way to live.
This brings us to one of the most transformative advancements in modern endocrinology: the insulin pump. If you have been researching ways to improve your metabolic control, you have likely come across this technology. But what are the medications for diabetes doing differently when delivered through a machine rather than a syringe?
As a board-certified endocrinologist, I spend a significant portion of my week helping patients transition from manual injections to automated technology.
This comprehensive 2026 guide will detail exactly what an insulin pump is, how these incredible devices work, their daily costs, and whether upgrading to one is the right clinical decision for your metabolic health.
What Is an Insulin Pump?
For those newly diagnosed or looking to upgrade their care, it is crucial to clearly define insulin pump technology. Simply put, an insulin pump is a small, computerized, wearable medical device designed to deliver continuous doses of fast-acting insulin into your body.
When my patients ask to have the insulin pump explained in simple terms, I describe it as an artificial pancreas. Instead of relying on you to manually inject insulin every time you eat or wake up with high blood sugar, the device automates much of the process.
What does an insulin pump mean for your daily routine? It means freedom from carrying pens and vials everywhere you go. In the medical community, what an insulin pump is is Continuous Subcutaneous Insulin Infusion (CSII) therapy, highlighting its role as a steady, uninterrupted lifeline.
What Is an Insulin Pump Used For?
The fundamental goal of diabetes management is to keep your blood glucose as close to a normal, non-diabetic range as safely possible. Therefore, what an insulin pump is used for primarily is achieving ultra-tight blood sugar control while minimizing the risk of severe hypoglycemia (low blood sugar).
What is the function of an insulin pump on a biological level? It aims to perfectly mimic the natural, drip-like insulin release of a healthy human pancreas. By providing a continuous baseline of insulin, it prevents the drastic peaks and valleys commonly experienced with traditional injection therapies.
What Is an Insulin Pump and How Does It Work?
Understanding what an insulin pump is and how it works removes the fear and mystery surrounding wearable medical tech. The device operates using a combination of highly precise micro-motors and sophisticated software algorithms. Here is how an insulin pump delivers its life-saving hormone.
Continuous Delivery (Basal Rate)
The most important feature of the device is its background delivery. What is a basal rate on an insulin pump? It is the tiny, continuous trickle of insulin the pump pushes into your body 24 hours a day, keeping your blood sugar stable between meals and overnight.
If you are wondering what the basal rate on an insulin pump is programmed to do, it essentially replaces the long-acting insulin shot (like Lantus) you would normally take once a day. Your endocrinologist will highly customize this rate to match your specific circadian rhythm.
Mealtime Doses (Bolus)
When you sit down to eat a meal containing carbohydrates, the background basal rate is not enough. You must use the pump interface to deliver a “bolus.” A bolus is a large, immediate surge of insulin designed to cover the specific amount of food you are about to consume.
Delivery System Setup
The pump does not just sit on your skin; it requires a physical connection to your bloodstream. This is achieved through a specialized tube and a tiny, flexible cannula inserted just under the fatty layer of your skin, ensuring the insulin absorbs smoothly and consistently.
Key Components of an Insulin Pump
To fully grasp the technology, you need to understand the individual parts that make the system function safely.
First is the main pump device, which houses the computer screen, the battery, and the mechanical motor. Inside this device sits the reservoir, which is a small, replaceable plastic cartridge that holds a two-to-three-day supply of liquid insulin.
Next is the delivery mechanism. What is an infusion set that insulin pump users rely on? It is the medical tubing that connects the pump’s reservoir to your body. Finally, you have the cannula. What is the cannula on an insulin pump? It is a microscopic, soft Teflon tube that sits painlessly under your skin to deliver the fluid. This is how the insulin pump attached to the body remains secure.
Insulin Pump Design & Appearance
Patients are often concerned about the aesthetics and bulkiness of medical devices. What does an insulin pump look like today? Modern pumps are incredibly sleek, typically resembling a small pager, a tiny smartphone, or an oversized wireless earbud case.
What does an insulin pump look like on a person? Most tubed devices are discreetly clipped to a belt, tucked into a pocket, or hidden in a specialized bra pouch. The insulin pump machine is designed to be as unobtrusive as possible, allowing users to play sports, sleep, and work without interference.
Types of Insulin Pumps
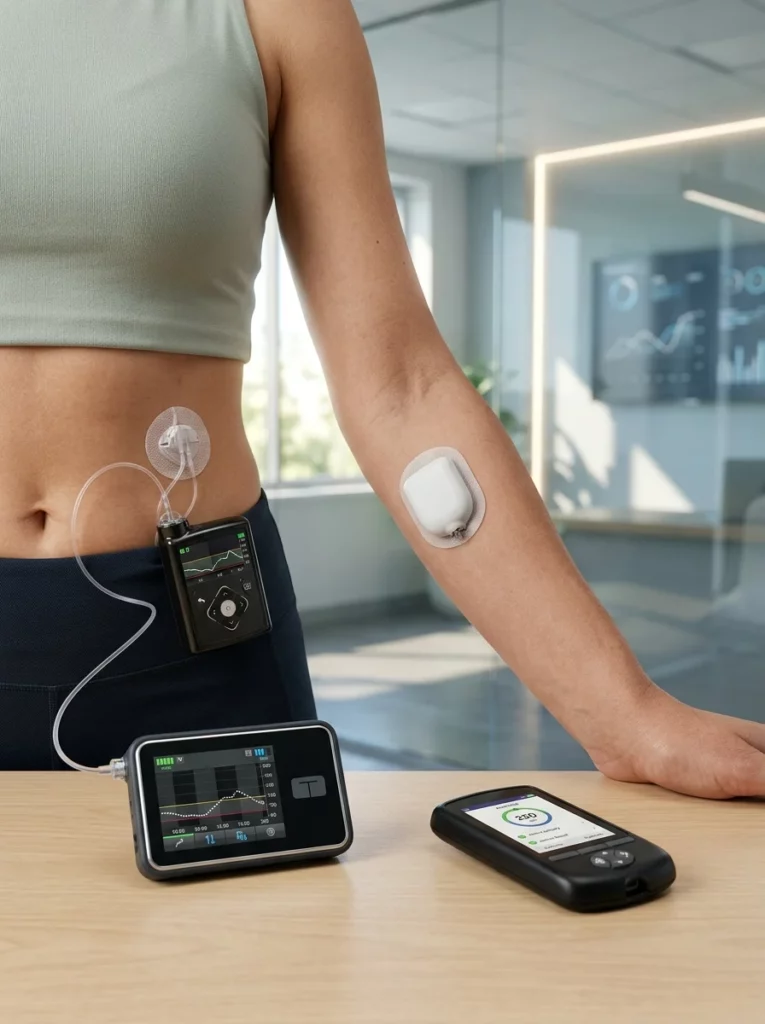
The technology landscape has exploded in recent years, offering patients unprecedented choices. When evaluating the types of diabetes medication delivery systems, you must understand that not all pumps are created equal. The market is primarily divided into two main categories, each serving different lifestyle needs.
Traditional Tubed Devices
Traditional insulin pumps are the oldest and most clinically established devices on the market. They consist of a durable external device (the pump itself) connected to the body via a long, flexible plastic tube. Brands like Medtronic and Tandem dominate this space.
The primary advantage of tubed pumps is their large insulin capacity and advanced integration with continuous glucose monitors (CGMs). They house incredibly smart algorithms, often referred to as “closed-loop” systems, which automatically adjust your basal rates every five minutes based on your real-time blood sugar readings.
However, the tubing can sometimes be a nuisance. It can accidentally catch on doorknobs or get tangled while sleeping. Despite this, they remain the gold standard for many endocrinologists due to their robust safety features, detailed data tracking, and easily readable external screens.
Wireless Patch Devices
For patients who absolutely refuse to wear medical tubing, patch pumps are a revolutionary alternative. These devices are completely tubeless. The entire system—the insulin reservoir, the cannula, and the pumping mechanism—is housed within a single, disposable, water-resistant pod that adheres directly to your skin.
What is an Omnipod insulin pump? The Omnipod is the most famous example of a patch pump. You fill the pod with insulin, stick it to your arm, stomach, or thigh, and control it wirelessly via a separate handheld device or a compatible smartphone app. Once the pod is empty (usually after three days), you throw the entire unit away and apply a new one.
Because of their simplicity, lack of tubes, and discreet profile, patch pumps are frequently considered the best insulin pumps for type 2 diabetes patients who are newly transitioning to pump therapy and want the least intrusive experience possible.
What Insulin Is Used in an Insulin Pump?
A very common misconception is that pumps use a mix of long and short-acting insulins. What insulin is in an insulin pump, actually? Pumps strictly use rapid-acting insulins, such as Humalog, Novolog, or Fiasp.
Because the pump continuously drips this fast-acting insulin into your body every few minutes, it artificially creates a long-acting “basal” effect. You never put thick, long-acting cloudy insulins into a pump, as they would clog the microscopic mechanics and disrupt the precise delivery algorithms.
Who Qualifies for an Insulin Pump?
Historically, insulin pumps were reserved exclusively for those with an autoimmune diagnosis. Therefore, when asking what an insulin pump for type 1 diabetes is, it is essentially the gold standard of modern care. Because type 1 patients produce zero insulin, the continuous delivery perfectly replaces their non-functioning pancreas.
However, the medical landscape is rapidly changing. What is an insulin pump for type 2 diabetes used for today? It is increasingly prescribed for type 2 patients who suffer from severe insulin resistance and require multiple daily injections to control their numbers.
Why would a patient need an insulin pump if they already use pens? The primary reason is unpredictable blood sugar swings. If you suffer from frequent hypoglycemia unawareness or a high A1C despite strict adherence to your pen injections, you are an ideal candidate.
Ultimately, who qualifies for an insulin pump depends on your endocrinologist’s assessment of your current glucose control, your willingness to learn the technology, and your insurance coverage.
Insulin Pump vs Insulin Pen
To understand why this technology is so revolutionary, we must compare it to the traditional method of delivery. What is an insulin pen? It is a manual, disposable device pre-filled with insulin that requires you to attach a needle and manually inject yourself for every single dose.
Here is a clear comparison of an insulin pump vs. an insulin pen:
| Feature | Insulin Pump | Insulin Pen |
| Delivery Method | Continuous, automated drip | Manual, individual injections |
| Injections Required | One site change every 3 days | 3 to 5 separate injections per day |
| Precision | Micro-doses (as little as 0.025 units) | Standard doses (usually whole or half units) |
| Flexibility | Extremely high (can pause or reduce delivery) | Moderate (once injected, it cannot be undone) |
| Data Tracking | Syncs with CGM, tracks active insulin | Manual logging required by the patient |
What Is an Advantage of an Insulin Pump?
The clinical benefits of transitioning to wearable technology are profound. What is an advantage of an insulin pump that patients notice first? The immediate reduction in needle fatigue. Instead of piercing your skin up to 150 times a month, a pump reduces that to roughly 10 site changes per month.
Another massive benefit is lifestyle flexibility. What is the advantage of an insulin pump when exercising or sleeping? If your blood sugar drops during a workout, you can simply press a button to temporarily suspend your insulin delivery—something impossible to do once you have injected a manual pen dose.
Furthermore, clinical studies consistently show that pump users achieve a lower, more stable A1C. The ability to give precise micro-doses for small snacks or slightly elevated sugars prevents the massive roller-coaster effect often seen with manual injections.
Disadvantages of Insulin Pump
Despite the life-changing benefits, the technology is not perfect. You must weigh the disadvantages of insulin pump therapy before committing. The most significant risk is a technical failure; if the tubing kinks or the battery dies, your insulin stops completely.
Because pumps only use fast-acting insulin, a delivery failure can lead to diabetic ketoacidosis (DKA) within mere hours. What is a disadvantage of an insulin pump regarding daily life? You are physically attached to a medical device 24/7, which can cause skin irritation or psychological burnout for some users.
What Is the Cost of an Insulin Pump?
Financial accessibility is the biggest barrier for most patients. What is the cost of an insulin pump without insurance? The initial retail price of the hardware (the pump itself) can range between $4,500 and $8,000.
However, the hardware is only part of the equation. How much does it cost per month to operate? You must purchase disposable infusion sets, reservoirs, and adhesive patches, which typically cost an additional $150 to $300 monthly.
Patients often ask, “What is the price of an insulin pump for patch devices like Omnipod?” Because there is no heavy upfront hardware cost, you pay a continuous monthly pharmacy subscription for the pods, averaging around $800 a month out-of-pocket.
Are insulin pumps free? No, but highly comprehensive health insurance plans or strict Medicare Part B criteria can cover up to 80% to 100% of the automatic insulin pump price if medical necessity is explicitly proven by your doctor.
How Are Insulin Pumps Installed?
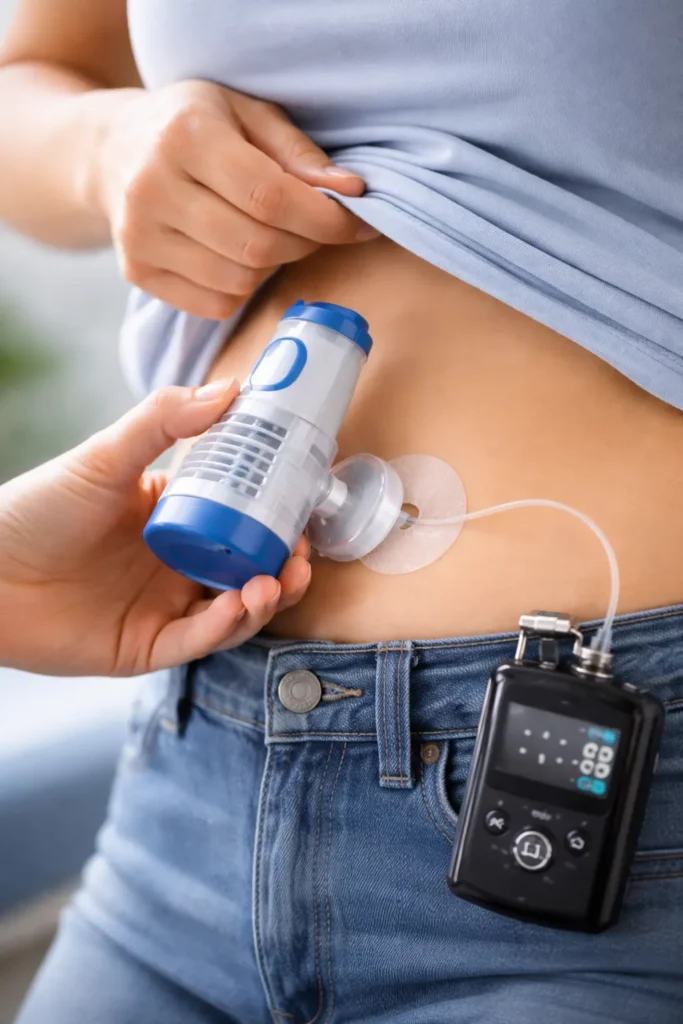
Switching to an insulin pump necessitates clinical training. How are insulin pumps applied to your body? You utilize a spring-loaded insertion device supplied by the manufacturer. By pressing it against your cleaned skin (typically the abdomen), you push a button, and a small needle inserts a soft cannula into your fatty tissue before retracting immediately.
You never actually feel a needle sitting inside you; only a tiny, flexible Teflon tube remains. Patients frequently ask, “Why do insulin pumps only last 3 days?” If you leave the cannula in longer, scar tissue begins to form, and the insulin will pool under the skin instead of properly absorbing into the bloodstream.
Using an Insulin Pump Day-to-Day
Living with a pump requires daily engagement. Your primary responsibility is monitoring your blood sugar, ideally through a connected continuous glucose monitor (CGM).
When you sit down for breakfast, you simply tell the pump exactly how many carbohydrates you are about to eat. The pump’s internal calculator computes your current blood sugar, your active insulin, and the meal size, delivering the perfect dose with the push of a button.
Every three days, you must engage in site maintenance. This involves drawing fresh insulin from a glass vial, filling a new plastic pump reservoir, removing your old infusion set, and deploying a new cannula on a different part of your body to let the old site heal.
Important Insulin Pump Settings
To safely operate this machinery, your endocrinologist will program highly specific mathematical formulas into the device’s brain.
The most critical settings are your basal rates (the background drip) and your insulin-to-carbohydrate ratios. Many advanced users also utilize established mathematical principles to adjust their own care.
What is the 500 rule for insulin pumps? It is a standard clinical formula used to determine your carbohydrate ratio. You divide the number 500 by your total daily dose of insulin. The resulting number tells you exactly how many grams of carbohydrates one single unit of rapid-acting insulin will safely cover.
Blood Sugar Management with Pumps
The ultimate goal of wearing this device is maintaining “Time in Range.” The ideal target for most patients is keeping their glucose between 70 mg/dL and 180 mg/dL for at least 70% of the day.
When monitoring their numbers, international patients often use the mmol/L measurement and ask, “Is 7.8 blood sugar too high?” A reading of 7.8 mmol/L (roughly 140 mg/dL) is actually an excellent, safe post-meal target, though it would be considered slightly elevated if you were completely fasting.
FAQs
What is an insulin pump?
An insulin pump is a small, computerized, wearable medical device that continuously delivers fast-acting insulin into the fatty tissue beneath the skin to regulate blood sugar levels.
How does an insulin pump work?
It works by delivering a continuous, micro-drip of background insulin (basal rate) 24 hours a day, alongside larger, on-demand surges of insulin (bolus) initiated by the user during meals.
What does an insulin pump look like?
Traditional tubed insulin pumps look like small pagers or thick smartphones with a digital screen, while wireless patch pumps look like small, white, plastic pods adhered directly to the skin.
Why would someone need an insulin pump?
A patient needs an insulin pump when traditional manual injections fail to provide stable blood sugar control, resulting in severe A1C elevation or dangerous, unpredictable drops in glucose.
How much does an insulin pump cost?
Without insurance, the initial pump device costs between $4,500 and $8,000, plus an ongoing $150 to $300 monthly fee for necessary disposable supplies like infusion sets and reservoirs.
Conclusion
Deciding to transition to an insulin pump is a profound step forward in managing your metabolic health. As we have explored in this complete 2026 guide, these advanced wearable devices offer unparalleled flexibility, precision, and freedom from the relentless cycle of daily manual injections.
While the technology requires a learning curve, financial investment, and daily attention, the clinical benefits of stabilized blood sugars and reduced complication risks are undeniable. An insulin pump does not cure diabetes, but it serves as a powerful, intelligent artificial pancreas that can help you reclaim a sense of normalcy in your life.
If you are struggling with unpredictable glucose swings or severe needle fatigue, do not settle for outdated care. Talk to your endocrinologist today to see if you qualify for this life-changing technology.
Medical Disclaimer: This article is written by a board-certified endocrinologist for educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Always consult your healthcare provider before changing your insulin delivery system or adjusting your medical dosages.
Authoritative Medical References:
- American Diabetes Association (ADA) – Diabetes Care Journal: Diabetes Technology
- The New England Journal of Medicine (NEJM)
- The Lancet Diabetes & Endocrinology
- National Institute of Diabetes and Digestive and Kidney Diseases (NIDDK): Insulin Resistance & Prediabetes
- Centers for Disease Control and Prevention (CDC): Insulin Resistance and Diabetes

